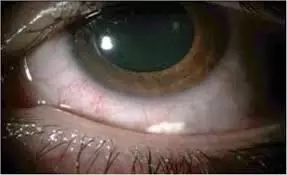
Subconjunctival triamcinolone acetonide injection useful prophylactic therapy for pseudophakic macular edema: Study
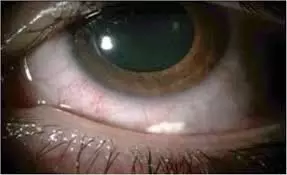
Subconjunctival triamcinolone acetonide injection useful prophylactic therapy for pseudophakic macular edema suggests a study published in the Ophthalmology.
A study was done to compare the effectiveness and safety of a single injection of subconjunctival triamcinolone acetonide (TA) with that of postoperative topical prednisolone acetate (PA) with and without nonsteroidal anti-inflammatory drugs (NSAIDs) for cataract surgery prophylaxis. Patients at Kaiser Permanente Northern California from 2018 through 2021. Exposure groups included topical PA with or without NSAID and subconjunctival injection of TA (Kenalog; Bristol-Myers-Squibb) 10 mg/ml or 40 mg/ml in a low dose (1.0-3.0 mg) or high dose (3.1-5.0 mg).The adjusted odds ratio (OR) and 95% confidence interval (CI) for the association of postoperative macular edema (ME) and iritis diagnoses 15 to 120 days after surgery (effectiveness measures) and a glaucoma-related event (safety measure) between 15 days and 1 year after surgery. Results: Of 69 832 eligible patient-eyes, postoperative ME, iritis, and a glaucoma-related event occurred on average in 1.3%, 0.8%, and 3.4% of eyes in the topical groups and 0.8%, 0.5%, and 2.8% of eyes in the injection groups, respectively. In multivariable analysis, compared with the PA reference group, the PA plus NSAID group had a lower OR of ME (OR, 0.88; 95% CI, 0.74-1.04; P = 0.135). and all injection groups had even lower odds, with the high-dose TA 10-mg/ml group reaching statistical significance (OR, 0.64; 95% CI, 0.43-0.97; P = 0.033). A trend of lower odds of a postoperative iritis diagnosis was noted in the high-strength (40 mg/ml) groups. For postoperative glaucoma-related events, compared with PA, the TA 10-mg/ml low-dose group showed lower odds (OR, 0.69; 95% CI, 0.55-0.86; P = 0.001), the TA 10-mg/ml high-dose group showed similar odds (OR, 0.90; 95% CI, 0.70-1.15; P = 0.40), and the TA 40-mg/ml low-dose and high-dose groups showed higher odds of an event occurring (OR, 1.46 [95% CI, 0.98-2.18; P = 0.062] and OR, 2.14 [95% CI, 1.36-3.37; P = 0.001], respectively). The TA 10-mg/ml high-dose (4 mg) group was associated with a lower risk of postoperative ME and a similar risk of glaucoma-related events compared with the topical groups.
Reference:
Shorstein NH, McCabe SE, Alavi M, Kwan ML, Chandra NS. Triamcinolone Acetonide Subconjunctival Injection as Stand-alone Inflammation Prophylaxis after Phacoemulsification Cataract Surgery. Ophthalmology. 2024 Oct;131(10):1145-1156. doi: 10.1016/j.ophtha.2024.03.025. Epub 2024 Apr 4. PMID: 38582155; PMCID: PMC11416342.
Keywords:
Subconjunctival, triamcinolone, acetonide, injection, prophylactic therapy, pseudophakic, macular, edema: Study, Shorstein NH, McCabe SE, Alavi M, Kwan ML, Chandra NS. Triamcinolone Acetonide Subconjunctival Injection, Ophthalmology, Dropless cataract surgery; Macular edema prophylaxis; Subconjunctival triamcinolone injection.