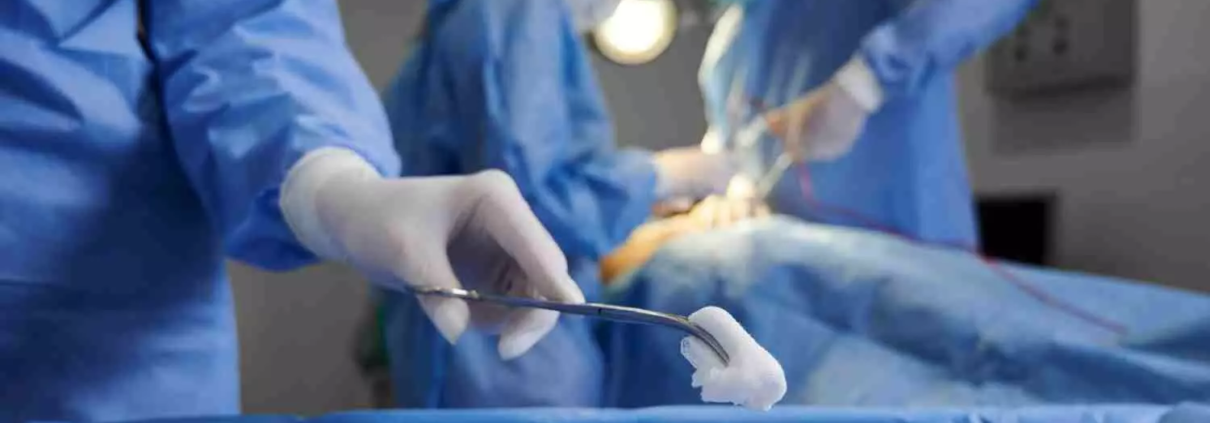
Frail elderly patients undergoing risky surgery more prone to Complications and mortality, finds study
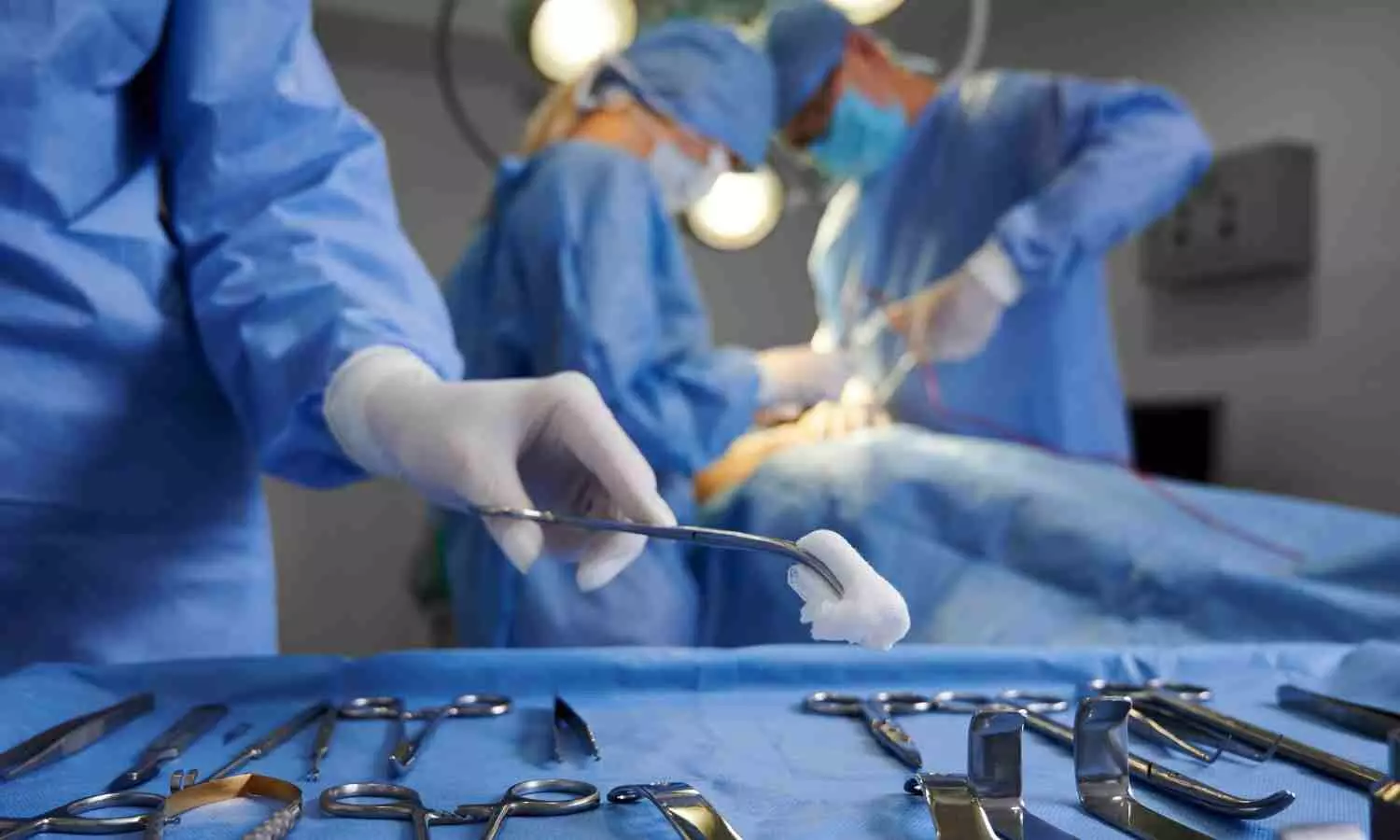
Frailty is a well-established predictor of complications and death after surgery. However, patients over 65 who undergo a high-risk operation in the emergency room are at significantly increased risk of postoperative complications and death in comparison to the same patients who are assessed solely on their level of frailty, according to a study published in the Journal of the American College of Surgeons (JACS).
In the United States, the elderly population is expected to double within the next 35 years. Emergency surgery for this population is challenging surgeons to consider more factors in decision making and plan for the most appropriate postoperative recovery.
“We are seeing a lot more elderly patients in the emergency department with acute surgical problems that require a major operation. And the outcomes for these individuals, compared to younger patients, are much worse,” said study co-author Raul Coimbra, MD, PhD, FACS, surgeon-in-chief of the Riverside University Health System in Moreno Valley, and a professor of surgery at Loma Linda University School of Medicine, both in California. “We need to counsel patients and their families about all the risks they are incurring when patients undergo a major emergency operation and be transparent about what to expect afterwards. Sometimes, the family believes the patient will return home. But in fact, a significant number of patients who have major surgery end up in nursing homes or rehab facilities and never go home.”
The researchers hypothesized that for the elderly population, the level of procedure risk (high or low) has a stronger impact on adverse outcomes when measured alongside frailty, compared with frailty status alone. Using the American College of Surgeons National Surgical Quality Improvement Program (ACS NSQIP), researchers examined the records of elderly patients (over age 65) who had undergone an emergency surgical procedure between 2018 and 2020. ACS NSQIP is the leading nationally validated, risk-adjusted, outcomes-based program to measure and improve the quality of surgical care in hospitals.
For the analysis, patients were classified as not frail, frail, and severely frail and then grouped according to procedure risk level — low-risk operations and high-risk operations. High-risk procedures included open cholecystectomy, open colectomy, laparoscopic colectomy, small bowel resection, and perforated ulcer repair. Low-risk procedures included appendectomies and cholecystectomies.
They then evaluated five outcomes-30-day mortality, 30-day postoperative complications, failure to rescue, hospital readmission, and 30-day reoperation. The purpose was to identify the impact of surgical procedure type on outcomes among elderly patients.
Key Findings
- Of the study’s 59,633 elderly patient sample, 29.3% were classified as non-frail, 66.4% as frail, and 4.3% as severely frail.
- Of those patients, 25,157 were in the low-risk procedure group and 34,476 in the high-risk procedure group.
- Frailty and procedure risk were both associated with increased risk of mortality, postoperative complications, failure to rescue, and readmissions. However, when patients were grouped according to procedure risk versus frailty alone, procedure risk proved to be a stronger link to adverse outcomes.
- For example, non-frail patients undergoing high-risk emergency surgical procedures had a 7.1% mortality rate, while the mortality rate of low-risk procedures was 0.2%. In contrast, frail and severely frail patients undergoing high-risk procedures had mortality rates of 11.5% and 25.8%, whereas mortality rates after low-risk procedures were 1.0% and 4.1%, respectively.
- Among non-frail patients, high-risk procedures accounted for a 4-fold increase in surgical complications compared to low-risk procedures. Similarly, high-risk procedures also accounted for a 4-fold increase in surgical complications among frail and severely frail patients.
- The difference between high-risk and low-risk procedures was at least four times greater in every outcome measure compared to frailty status alone. For instance, undergoing a high-risk procedure led to an 8-fold increase in 30-day mortality. In contrast, being severely frail resulted in a 3-fold increase in death within 30 days.
“What we also learned in this study is that a very significant number of elderly patients are coming to the emergency room for a major operation, urgently. And the reason is because elderly patients may not seek surgical care early on, and surgeons often shy away from solving the problems electively,” Dr. Coimbra said. “The problem is that diseases don’t disappear. They stay and progress and advance until these patients end up in the emergency department requiring an emergency operation.”
For elderly patients, putting off minor surgery may be detrimental to their long-term health and quality of life. The study authors hope these results will help shape new thinking about treating elderly patients earlier and about having more informed discussions with patients and their families about what to expect following emergency general surgery.
“The message from our study is that elderly patients should undergo surgical treatment when they first present with their disease. It should not be put off until complications develop to the point where an emergency operation is needed. Because that emergency operation is the most significant risk for mortality and complications,” he adds.
A major limitation of the study is that it is a retrospective study. Another limitation is that frailty is classified retrospectively. A more standardized description of frailty might have impacted the study’s findings.
Reference:
Zakhary, Bishoy BA, MPHa; Coimbra, Bruno C BSa,b; Kwon, Junsik MDa,c; Allison-Aipa, Timothy PhDa; Firek, Matthew BSa; Coimbra, Raul MD, PhD, FACSa,d,e. Procedure Risk vs Frailty in Outcomes for Elderly Emergency General Surgery Patients: Results of a National Analysis. Journal of the American College of Surgeons ():10.1097/XCS.0000000000001079, April 25, 2024. | DOI: 10.1097/XCS.0000000000001079.