Study reveals diet as main risk factor for colon cancer in younger adults
Powered by WPeMatico
Powered by WPeMatico
Powered by WPeMatico

New Delhi: Announcing the details of this year’s list of best pharmacy institutes across the country, the Union Education Minister Dharmendra Pradhan has released the National Institutional Ranking Framework (NIRF) 2024. Besides pharmacy, the rankings have been released under various categories including Overall, Medical, Engineering, Management, Pharmacy, Colleges, Architecture, Law, Dental and Research.
According to the National Institutional Ranking Framework, the Jamia Hamdard , New Delhi (JHU, New Delhi) maintains its record and ranks first in the pharmacy colleges list. The score of Jamia Hamdard has been increased from 78.74 in 2023 to 84.01 in 2024.
The rank of National Institute of Pharmaceutical Education and Research Hyderabad (NIPER, Hyderabad) has come down from rank Ist to rank 2nd in 2024 with a score of 80.29.
The Birla Institute of Technology and Science, Pilani Rajasthan has ranked 3rd in the pharmacy colleges list with a score of 78.95.
The 4th, 5th and 6th positions have been reserved by JSS College of Pharmacy, Tamilnadu and Institute of Chemical Technology Maharashtra, JSS College of Pharmacy Karnataka respectively.
The list of Top 100 pharmacy colleges as per NIRF 2024 has been given below:
| Rank | Name | State | Score |
| 1 | Jamia Hamdard | Delhi | 84.01 |
| 2 | National Institute of Pharmaceutical Education and Research Hyderabad |
Telangana | 80.29 |
| 3 | Birla Institute of Technology and Science, Pilani |
Rajasthan | 78.95 |
| 4 | JSS College of Pharmacy |
Tamil Nadu | 77.13 |
| 5 | Institute of Chemical Technology |
Maharashtra | 74.69 |
| 6 | JSS College of Pharmacy |
Karnataka | 72.89 |
| 7 | Panjab University | Chandigarh | 72.76 |
| 8 | Manipal College of Pharmaceutical Sciences, Manipal |
Karnataka | 72.27 |
| 9 | National Institute of Pharmaceutical Education and Research Mohali |
Punjab | 70.86 |
| 10 | SVKM`s Narsee Monjee Institute of Management Studies |
Maharashtra | 69.94 |
| 11 | S.R.M. Institute of Science and Technology |
Tamil Nadu | 68.90 |
| 12 | National Institute of Pharmaceutical Education and Research Guwahati |
Assam | 68.82 |
| 13 | Amrita Vishwa Vidyapeetham |
Tamil Nadu | 68.07 |
| 14 | National Institute of Pharmaceutical Education and Research Raebareli |
Uttar Pradesh | 65.53 |
| 15 | National Institute of Pharmaceutical Education and Research Ahmedabad |
Gujarat | 64.89 |
| 16 | Delhi Pharmaceutical Sciences and Research University |
Delhi | 64.73 |
| 16 | Lovely Professional University |
Punjab | 64.73 |
| 18 | Jadavpur University | West Bengal | 64.14 |
| 19 | Chitkara University | Punjab | 64.05 |
| 20 | Chandigarh University | Punjab | 64.01 |
| 21 | Babasaheb Bhimrao Ambedkar University |
Uttar Pradesh | 61.78 |
| 22 | Amity University | Uttar Pradesh | 61.07 |
| 23 | Central University of Punjab |
Punjab | 60.92 |
| 24 | National Institute of Pharmaceutical Education and Research Kolkata |
West Bengal | 58.76 |
| 25 | I. S. F. College of Pharmacy |
Punjab | 58.27 |
| 26 | Maharishi Markandeshwar (Deemed to be University) |
Haryana | 58.24 |
| 27 | Annamalai University | Tamil Nadu | 58.19 |
| 28 | Banasthali Vidyapith | Rajasthan | 57.77 |
| 29 | Central University of Rajasthan |
Rajasthan | 57.65 |
| 30 | Shoolini University of Biotechnology and Management Sciences |
Himachal | 57.07 |
| 31 | Sri Ramachandra Institute of Higher Education and Research |
Tamil Nadu | 56.98 |
| 32 | Birla Institute of Technology |
Jharkhand | 56.75 |
| 33 | National Institute Of Pharmaceutical Education And Research Hajipur |
Bihar | 56.40 |
| 34 | AU College of Pharmaceutical Sciences, Andhra University |
Andhra Pradesh | 56.11 |
| 35 | Poona College of Pharmacy, Pune |
Maharashtra | 55.86 |
| 36 | Dr D Y Patil Institute of Pharmaceutical Sciences and Research |
Maharashtra | 55.24 |
| 37 | Nirma University | Gujarat | 55.22 |
| 38 | Maharshi Dayanand University |
Haryana | 54.53 |
| 39 | SVKM`s Dr. Bhanuben Nanavati College of Pharmacy |
Maharashtra | 54.18 |
| 40 | Noida Institute of Engineering and Technology (Pharmacy Institute) |
Uttar Pradesh | 53.55 |
| 41 | N.G.S.M. Institute of Pharmaceutical Sciences |
Karnataka | 53.35 |
| 42 | KLE College of Pharmacy, Belgaum |
Karnataka | 52.66 |
| 43 | Dibrugarh University | Assam | 52.16 |
| 44 | Maharaja Sayajirao University of Baroda |
Gujarat | 51.93 |
| 45 | Integral University | Uttar Pradesh | 51.44 |
| 46 | Punjabi University | Punjab | 51.33 |
| 47 | Parul University | Gujarat | 51.30 |
| 48 | Gandhi Institute of Technology and Management |
Andhra Pradesh | 51.03 |
| 49 | Suresh Gyan Vihar University |
Rajasthan | 50.81 |
| 50 | Galgotias University | Uttar Pradesh | 50.73 |
| 51 | Rashtrasant Tukadoji Maharaj Nagpur University |
Maharashtra | 50.22 |
| 52 | L. M. College of Pharmacy |
Gujarat | 50.02 |
| 53 | G. L. A. University | Uttar Pradesh | 49.74 |
| 54 | Guru Ghasidas Vishwavidyalaya |
Chhattisgarh | 49.65 |
| 55 | Guru Jambheshwar University of Science and Technology |
Haryana | 48.98 |
| 56 | R. C. Patel Institute of Pharmaceutical Education and Research |
Maharashtra | 48.75 |
| 57 | Amar Shaheed Baba Ajit Singh Jujhar Singh Memorial College |
Punjab | 48.51 |
| 58 | PSG College of Pharmacy |
Tamil Nadu | 48.08 |
| 59 | Mohan Lal Sukhadia University |
Rajasthan | 47.03 |
| 60 | Sri Padmavathi Mahila Visvavidyalayam |
Andhra Pradesh | 46.63 |
| 61 | Smt. Kishoritai Bhoyar College of Pharmacy |
Maharashtra | 46.37 |
| 62 | Kumaun University, Nainital |
Uttarakhand | 46.34 |
| 63 | Acharya Nagarjuna University College of Pharmaceutical Sciences |
Andhra Pradesh | 46.10 |
| 64 | Vels Institute of Science Technology and Advanced Studies (VISTAS) |
Tamil Nadu | 46.00 |
| 65 | Nandha College of Pharmacy |
Tamil Nadu | 45.50 |
| 66 | Chandigarh College of Pharmacy |
Punjab | 45.30 |
| 67 | Krishna Vishwa Vidyapeeth |
Maharashtra | 45.13 |
| 68 | M.S. Ramaiah University of Applied Sciences |
Karnataka | 45.02 |
| 69 | Sharda University | Uttar Pradesh | 44.75 |
| 70 | Gujarat Technological University |
Gujarat | 44.33 |
| 71 | Anurag University | Telangana | 44.22 |
| 72 | Dr. Vishwanath Karad MIT World Peace University |
Maharashtra | 43.74 |
| 73 | Bombay College of Pharmacy |
Maharashtra | 43.72 |
| 74 | Guru Nanak Institute of Pharmaceutical Science and Technology |
West Bengal | 43.66 |
| 74 | Bundelkhand University |
Uttar Pradesh | 43.66 |
| 76 | Y. B. Chavan College of Pharmacy |
Maharashtra | 43.49 |
| 77 | KIET Group of Institutions: KIET Group of Pharmacy |
Uttar Pradesh | 43.42 |
| 78 | College of Pharmacy, Madras Medical College |
Tamil Nadu | 43.36 |
| 79 | Sri Venkateswara College of Pharmacy |
Andhra Pradesh | 42.77 |
| 80 | Bharati Vidyapeeth College of Pharmacy |
Maharashtra | 42.50 |
| 81 | DIT University | Uttarakhand | 42.48 |
| 82 | Arulmigu Kalasalingam College of Pharmacy |
Tamil Nadu | 41.58 |
| 83 | Sri Adichunchanagiri College of Pharmacy |
Karnataka | 41.54 |
| 84 | B. S. Abdur Rahman Crescent Institute of Science and Technology |
Tamil Nadu | 41.48 |
| 85 | Sam Higginbottom Institute of Agriculture, Technology and Sciences |
Uttar Pradesh | 41.45 |
| 86 | Acharya & B M Reddy College of Pharmacy |
Karnataka | 41.35 |
| 87 | Vishnu Institute of Pharmaceutical Education and Research |
Telangana | 41.19 |
| 88 | Kakatiya University | Telangana | 41.15 |
| 89 | Vinayaka Mission’s Research Foundation |
Tamil Nadu | 41.01 |
| 90 | Ramanbhai Patel College of Pharmacy |
Gujarat | 40.90 |
| 91 | Uka Tarsadia University, Bardoli |
Gujarat | 40.87 |
| 92 | Shri Vishnu College of Pharmacy |
Andhra Pradesh | 40.72 |
| 93 | Goa College of Pharmacy |
Goa | 40.69 |
| 94 | Dr. B. C. Roy College of Pharmacy and Allied Health Sciences |
West Bengal | 40.67 |
| 95 | CMR College of Pharmacy |
Telangana | 40.51 |
| 96 | P. E. Society`s Modern College of Pharmacy |
Maharashtra | 40.30 |
| 97 | Principal K.M. Kundnani College of Pharmacy |
Maharashtra | 40.23 |
| 98 | Krupanidhi College of Pharmacy |
Karnataka | 40.10 |
| 99 | AISSMS College of Pharmacy |
Maharashtra | 39.97 |
| 100 | College of Pharmacy, Pandit Bhagwat Dayal Sharma University of Health Sciences |
Haryana | 39.54 |
Union Minister for Education Shri Dharmendra Pradhan recently released the India Rankings 2024, which implements the National Institutional Ranking Framework (NIRF) drafted for this purpose by the Ministry of Education in 2015. Secretary, Higher Education, Shri K. Sanjay Murthy; UGC, Prof. M Jagadesh Kumar; Chairman, AICTE, Prof. T.G. Sitharam; Chairman, NETF, Prof. Anil Sahasrabuddhe; Member Secretary, NBA, Dr. Anil Kumar Nassa, Additional Secretary, Department of Higher Education, Shri Sunil Kumar Barnwal; Joint Secretary, Shri Govind Jaiswal; Chairman, and other academicians, heads of the institutions, etc. were present on this occasion.
Shri Dharmendra Pradhan while addressing the audience said that Rankings, ratings and accreditation is a vital recommendation of NEP 2020. It is heartening that NIRF rankings deeply reflect the spirit of NEP, he added. The Minister congratulated all the HEIs who have demonstrated excellence in teaching, innovation, research, graduation outcomes and other parameters and bagged a place of pride in the India Rankings 2024.
The Minister stressed that knowing the quality, performance and strengths of an academic institution is a right of students and parents. Therefore, all the 58,000 HEIs in the country must come under the ranking and rating framework. Shri Pradhan stated that employability and skills are a priority. He also said that our ranking mechanism must also include skilling as a parameter. Intangible aspects are powerful stimulus to learning and development. We should devise mechanisms to bring intangible aspects of education in the rankings framework, he added.
Five Broad Categories of Parameters and Weightage
The National Institutional Ranking Framework (NIRF), launched in November 2015 by the Ministry of Education, was used for this edition as well as for the previous eight editions of India Rankings released for the years 2016 to 2023. Five broad categories of parameters identified in the NIRF and their weightage on scale of 10 are given below:
|
Sl. No. |
Parameter |
Marks |
Weightage |
|
1 |
Teaching, Learning & Resources |
100 |
0.30 |
|
2 |
Research and Professional Practice |
100 |
0.30 |
|
3 |
Graduation Outcome |
100 |
0.20 |
|
4 |
Outreach and Inclusivity |
100 |
0.10 |
|
5 |
Perception |
100 |
0.10 |
Each of these five parameters have 2 to 5 sub-parameters. A total number of 18 parameters are used for ranking of HEIs in different categories and subject domains. Institutions are ranked based on total sum of marks assigned for each of these five broad groups of parameters.
Besides, sourcing data on various parameters from applicant institutions, third party sources of data have also been used, wherever possible. Scopus (Elsevier Science) and Web of Science (Clarivate Analytics) were used for retrieving publications and citations data. Derwent Innovation was used for retrieving data on patents. Data retrieved from these sources was shared with the institutions for transparency with a provision to give their inputs.
The Minister urged to all the captains of Indian academia to come under the ranking framework, set ambitious goals and strive for higher rankings in future editions. Together, let’s foster an environment of educational excellence for realising the goal of Viksit Bharat, he added.
Powered by WPeMatico

Nagpur: The AYUSH doctors across the
state are criticizing a new policy introduced by the Maharashtra Council of
Indian Medicines (MCIM). The mandate requires these practitioners to renew
their registrations by earning credits through an MCIM-affiliated online
Continuing Medical Education (CME) platform, which could cost them up to
₹50,000 over a span of five years.
The proposed policy stipulates
that AYUSH doctors must accumulate 50 credit points to renew their
registration. Of these, a minimum of 30 points must be earned via an online CME
platform affiliated with MCIM, while the remaining 20 points can be gathered
through traditional CME programs. The online platform, managed by a private firm,
is charging ₹1,100 per lecture, raising concerns among the doctors about the
financial burden this places on them.
AYUSH doctors have voiced strong
objections to this mandate, alleging that the process is riddled with
irregularities. Many are calling for a review of the policy, citing the high
costs and questioning the fairness and transparency of the system. As the debate
intensifies, the medical community is urging the authorities to reconsider the
financial implications of this new requirement on the state’s AYUSH
practitioners.
Talking to Medical Dialogues, Dr Mohan Yende, general secretary of the National Integral Medical Association (NIMA),
Maharashtra stated, “Before 2019 the renewal used to cost Rs 50 only; however,
in 2019 MCM increased the registration cost to Rs. 2000 for 5 years. NIMA
challenged the new rules in Mumbai High Court and the case is still going on. The
national body of registration regulation amended its rules in October 2023 and stated that all doctors should score 50 credit points for their
upgradation of medical knowledge.”
“However, to access the videos, the
doctors have to pay Rs. 1100 per video and this is preposterous. We have no
problem gaining more academic knowledge through the system of credit points but
imposing this hefty sum on the doctors cannot be accepted, especially
considering that they are serving pre-recorded videos and the session is not
interactive. They should have surveyed the matter properly or communicated with
different doctors’ organizations before drafting such a new policy,” he added.
Powered by WPeMatico

Cambridge: AstraZeneca and Daiichi Sankyo’s Enhertu (trastuzumab deruxtecan) has received conditional approval in China as a monotherapy for the treatment of adult patients with locally advanced or metastatic HER2-positive gastric or gastroesophageal junction (GEJ) adenocarcinoma who have received two or more prior treatment regimens.
The conditional approval by the National Medical Products Administration (NMPA) was based on the positive results of the DESTINY-Gastric06 Phase II trial. Full approval for this indication will depend on whether a randomised controlled confirmatory clinical trial can demonstrate clinical benefit in this population.
Enhertu is a specifically engineered HER2-directed antibody drug conjugate (ADC) discovered by Daiichi Sankyo and being jointly developed and commercialised by AstraZeneca and Daiichi Sankyo.
In the DESTINY-Gastric06 trial, Enhertu demonstrated clinically meaningful efficacy in patients in China with locally advanced or metastatic HER2-positive gastric or GEJ adenocarcinoma previously treated with two or more prior regimens including a fluoropyrimidine agent and a platinum agent.
More than one third of the global cases of gastric cancer occur in China, with about 65% of patients presenting with advanced disease at the time of diagnosis. Approximately 359,000 new cases of gastric cancer and 260,000 deaths were reported in China in 2022. Roughly one in five gastric cancers globally are HER2-positive.
Lin Shen, MD, Director of the Department of Gastrointestinal Oncology, Peking University Cancer Hospital, China, said, “HER2-positive metastatic gastric cancer can be particularly aggressive and difficult to treat. Patients often face poor outcomes following disease progression on first-line treatment and subsequent chemotherapy. With the approval of Enhertu, patients in China with HER2-positive metastatic gastric cancer will now have an important anti-HER2 treatment option that has demonstrated clinically meaningful efficacy following progression on previous therapies.”
Dave Fredrickson, Executive Vice President, Oncology Business Unit, AstraZeneca, said, “China accounts for more than a third of patients with gastric cancer globally and most patients are diagnosed with advanced disease. This approval of Enhertu brings a much-needed, new targeted treatment option to patients with HER2-positive metastatic gastric cancer in China and underscores our commitment to bringing this innovative medicine to more patients across the globe living with HER2-expressing cancers.”
Kiminori Nagao, Head of the Asia, South & Central America Business Unit, Daiichi Sankyo, said, “This milestone marks the third approval in China for Enhertu in less than two years, following approvals for HER2-positive metastatic breast cancer and HER2-low metastatic breast cancer. Our DESTINY clinical trial programme continues to reinforce Enhertu as a practice-changing treatment option for patients with HER2-expressing cancers and this latest approval in China further illustrates the global impact of this innovative antibody drug conjugate.”
In DESTINY-Gastric06, treatment with Enhertu (6.4mg/kg) resulted in a confirmed objective response rate (ORR) of 28.8% as assessed by independent central review. Median progression-free survival (PFS) was 5.7 months.
The safety profile of Enhertu in DESTINY-Gastric06 was consistent with previous clinical trials of Enhertu in gastric cancer with no new safety concerns identified.
The approval was also supported by results from the DESTINY-Gastric01 Phase II trial which included patients from Japan and South Korea. In the trial, patients with HER2-positive metastatic gastric cancer treated with Enhertu showed a statistically significant improvement in confirmed ORR (40.5% with Enhertu versus 11.3% with chemotherapy; p<0.0001) and median overall survival (OS) (12.5 months with Enhertu versus 8.4 months with chemotherapy; hazard ratio [HR] 0.59; 95% confidence interval [CI] 0.39-0.88; p=0.0097).
Enhertu is already approved for advanced or metastatic gastric cancer in more than 45 countries, including the US, Japan and across the EU.
Read also: CDSCO panel approves AstraZeneca’s proposal for Amendment in Package Insert for Saxagliptin tablets
Powered by WPeMatico

Pandharpur: In a major development to advance healthcare facilities, Public Health Minister Tanaji Sawant announced the construction of a state-of-the-art 1,000-bed hospital in Pandharpur on Thursday. This project is designed to significantly enhance the region’s healthcare infrastructure and improve patient care facilities.
A prominent pilgrimage destination, Pandharpur located in Maharastra is known for its association with the Vithoba (vittala) deity a form of Lord Vishnu. The town attracts millions of devotees worldwide annually with numbers swelling especially during the Ashadi and Kartik Wari processions. The Wari processions are deeply rooted in tradition and reflect the spiritual zeal and devotion of the people.
Also Read: Sassoon General Hospital reels under shortage of staff, medicines, funds
However, the sub-district hospital cannot provide healthcare facilities to the devotees. This development is set to fill a critical gap in the region’s healthcare system.
In response to the issue, Minister Tanaji Sawant has requested Chief Minister Eknath Shinde to set up a hospital in Pandharpur to enhance the healthcare facility of the region. The Chief Minister agreed to this request, and a government resolution to this effect was issued on Thursday.
As per a media report in the HT, addressing the healthcare facility Sawant said, “This hospital is expected to provide significant benefits not only to the residents of Pandharpur and its surrounding areas but also to the millions of pilgrims who visit during the Wari festivals. The construction of this facility is anticipated to begin shortly and represents a major advancement in healthcare services for Pandharpur.”
Sawant informed that the new hospital will feature a comprehensive range of medical services, including emergency care, surgical facilities, specialized treatments, and outpatient, and inpatient departments. The Plans include advanced diagnostic equipment including laboratories and X-ray facilities. The facility also offers modern operating theatres, and dedicated wards to cater to various medical needs. The establishment of this large hospital will improve accessibility and quality of care for the local population.
Also Read: NBCC to build new medical college and 430 bedded hospital in Maharashtra
Powered by WPeMatico

New Delhi: India has altogether 31053 Primary Health Centres (PHCs), 6064 Community Health Centres (CHCs), 1275 Sub Divisional Hospitals, 767 District Hospitals, and 315 Government Medical Colleges, the Union Minister of State for Health Smt. Anupriya Patel recently informed the Lok Sabha.
The MoS Health also provided the details regarding the availability of health workers, AYUSH doctors, Allopathic practitioners, Pharmacists, Laboratory Technicians, and Nursing Staff at the PHCs and CHCs across the country.
This data was shared by the Union Health Ministry while responding to a question raised by Parliament member Shri Rajesh Verma, who sought to know the number of PHCs, CHCs, SDHs, DHs, and Union Government hospitals in the States/UTs as uploaded on the HMIS portal. He also questioned about the number of doctors, nurses, Health workers, and allied health professionals employed in Central Government operated hospitals and in other medical establishments and sought to know about the data regarding the vacant posts.
Apart from this, Shri Rajesh Verma also asked the Ministry about the steps taken/proposed to improve the number and quality of medical professionals in the public health system.
In response to these questions, the Union MoS Health provided the State/UT wise break up of PHCs, CHCs, SDHs, DHs, and MCs including Central Government Hospitals as per the Rural Health Statistics 2021-2022.
Availabiliity of PHCs:
As per the data provided by the Health Ministry, the maximum number of PHCs are in Uttar Pradesh, where 3513 PHCs are catering to the Public Health Sector.
Further, there are more than 1000 PHCs in States including Andhra Pradesh (1689), Assam (1010), Bihar (1760), Gujarat (1804), Karnataka (2521), Madhya Pradesh (1572), Maharashtra (2539), Odisha (1393), Rajasthan (2409), Tamil Nadu (1886), and West Bengal (1371).
Apart from these, there are 131 PHCs in Arunachal Pradesh, 822 in Chhatisgarh, 497 PHCs in Haryana, 570 in Himachal Pradesh, 361 PHCs in Jharkhand, 944 in Kerala, 147 in Meghalaya, 136 PHCs in Nagaland, 522 in Punjab, 834 PHCs in Telangana, 117 PHCs in Tripura, 607 in Uttarakhand, 550 PHCs in Delhi, and 973 in Jammu and Kashmir.
Less than 100 PHCs are available in States/UTs including Goa (28), Manipur (95), Mizoram (66), Sikkim (26), Andaman & Nicobar Islands (27), Chandigarh (43), Dadra & Nagar Haveli and Daman & Diu (14), Ladakh (33), Lakshadweep (4) and Puducherry (39).
Availabiliity of CHCs:
Among 6064 CHCs the maximum number of CHCs are available in Uttar Pradesh, where there are 841 Community Health Centres. Apart from this, there are 181 CHCs in Andhra Pradesh, 201 CHCs in Assam, 301 CHCs in Bihar, 170 CHCs in Chhattisgarh, 361 CHCs in Gujarat, 131 CHCs in Haryana, 178 CHCs in Jharkhand, 212 CHCs in Karnataka, 230 in Kerala, 356 in Madhya Pradesh, 398 in Maharashtra, 384 in Odisha, 160 in Punjab, 685 in Rajasthan, 400 in Tamil Nadu, and 348 in West Bengal.
States/UTs that have less than 100 CHCs include, Arunachal Pradesh (57), Goa (6), Himachal Pradesh (97), Manipur (17), Meghalaya (28), Mizoram (9), Nagaland (23), Sikkim (2), Telangana (82), Tripura (23), Uttarakhand (80), Andaman and Nicobar Islands (4), Chandigarh (2), Dadra & Nagar Haveli (4), Jammu & Kashmir (79), Ladakh (7), Lakshadweep), and Puducherry (4). There are no CHCs in Delhi.
Availability of Sub Divisional Hospitals:
The data revealed that among the 1275 Sub Divisional Hospitals, the maximum number i.e. 282 SDHs are available in Tamil Nadu. More than 100 SDHs are available in States/UTs including Karnataka (147), Madhya Pradesh (119). There are more than 50 SDHs available in Andhra Pradesh (51), Gujarat (54), Himachal Pradesh (84), Kerala (87), Maharashtra (93), and West Bengal (60).
Further, there are 14 SDHs in Assam, 45 in Bihar, 12 in Chhatisgarh, 24 in Haryana, 13 in Jharkhand, 33 in Odisha, 41 in Punjab, 22 in Rajasthan, 41 in Telangana, 12 in Tripura, and 19 SDHs n Uttarakhand.
States/UTs that have 10 or less than 10 SDHs include Goa (2), Manipur (1), Meghalaya (2), Mizoram (2), Sikkim (1), Chandigarh (1), Dadra & Nagar Haveli and Daman & Diu (1), Delhi (10), Lakshadweep (2).
Arunachal Pradesh, Nagaland, Uttar Pradesh, Andaman & Nicobar Islands, Jammu and Kashmir, Ladakh and Puducherry do not have Sub Divisional Hospitals.
Availability of District Hospitals:
As per the data shared by MoS Health, India has altogether 767 District Hospitals. Among these, the highest number i.e. 169 District Hospitals are available in Uttar Pradesh.
Apart from this, more than 30 District Hospitals are available in Kerala (48), Madhya Pradesh (52), Delhi (40), Bihar (36), Odisha (32), Rajasthan (30). Further, there are 25 District Hospitals in Assam, 27 in Chhattisgarh, 22 in Haryana, 21 in Jharkhand, 23 in Maharashtra, 23 in Punjab,
Less than 20 District Hospitals are in States/UTs including Goa (2), Himachal Pradesh (9), Manipur (7), Andhra Pradesh (17), Arunachal Pradesh (19), Gujarat (20), Meghalaya (11), Mizoram (12), Nagaland (12), Sikkim (4), Tamil Nadu (20), Telangana (5), Tripura (7), Uttarakhand (13), West Bengal (18), Andaman & Nicobar Islands (2), Chandigarh (1), Dadra & Nagar Haveli and Daman & Diu (2), Jammu and Kashmir (15), Ladakh (2), Lakshadweep (1), Puducherry (4).
More than 100 SDHs are available in States/UTs including Karnataka (147), Madhya Pradesh (119).
Availability of Medical Colleges:
Among the 315 medical colleges including central government hospitals available in India, the highest number of colleges i.e. 41 colleges are available in Tamil Nadu, followed by 40 medical colleges in Rajasthan.
More than 10 medical colleges are available in States/UTs including Andhra Pradesh (12), Bihar (11), Gujarat (20), Karnataka (19), Madhya Pradesh (13), Maharashtra (23), Uttar Pradesh (20), West Bengal (18), and Delhi (13).
States/UTs that have less than 10 medical colleges include Arunchal Pradesh (1), Assam (8), Chhattisgarh (8), Goa (1), Haryana (5), Himachal Pradesh (6), Jharkhand (7), Kerala (8), Manipur (2), Meghalaya (1), Mizoram (1), Odisha (7), Punjab (3), Telangana (9), Tripura (1), Uttarakhand (3), Andaman & Nicobar Islands (1), Chandigarh (2), Dadra & Nagar Haveli and Daman & Diu (1), Jammu and Kashmir (8), and Puducherry (2).
|
State/ UT wise number of PHCs, CHCs, SDHs, DHs & MC (including Central Government Hospitals) as reported by States/ UTs |
||||||
|
S. No. |
State/UTs |
Primary Health Centres (PHCs) |
Community Health Centres (CHCs) |
Sub Divisional Hospital (SDH) |
District Hospital (DH) |
Medical Colleges |
|
1 |
Andhra Pradesh |
1689 |
181 |
51 |
17 |
12 |
|
2 |
Arunachal Pradesh |
131 |
57 |
0 |
19 |
1 |
|
3 |
Assam |
1010 |
201 |
14 |
25 |
8 |
|
4 |
Bihar |
1760 |
301 |
45 |
36 |
11 |
|
5 |
Chhattisgarh |
822 |
170 |
12 |
27 |
8 |
|
6 |
Goa |
28 |
6 |
2 |
2 |
1 |
|
7 |
Gujarat |
1804 |
361 |
54 |
20 |
20 |
|
8 |
Haryana |
497 |
131 |
24 |
22 |
5 |
|
9 |
Himachal Pradesh |
570 |
97 |
84 |
9 |
6 |
|
10 |
Jharkhand |
361 |
178 |
13 |
21 |
7 |
|
11 |
Karnataka |
2521 |
212 |
147 |
16 |
19 |
|
12 |
Kerala |
944 |
230 |
87 |
48 |
8 |
|
13 |
Madhya Pradesh |
1572 |
356 |
119 |
52 |
13 |
|
14 |
Maharashtra |
2539 |
398 |
93 |
23 |
23 |
|
15 |
Manipur |
95 |
17 |
1 |
7 |
2 |
|
16 |
Meghalaya |
147 |
28 |
2 |
11 |
1 |
|
17 |
Mizoram |
66 |
9 |
2 |
12 |
1 |
|
18 |
Nagaland |
136 |
23 |
0 |
12 |
0 |
|
19 |
Odisha |
1393 |
384 |
33 |
32 |
7 |
|
20 |
Punjab |
522 |
160 |
41 |
23 |
3 |
|
21 |
Rajasthan |
2409 |
685 |
22 |
30 |
40 |
|
22 |
Sikkim |
26 |
2 |
1 |
4 |
0 |
|
23 |
Tamil Nadu |
1886 |
400 |
282 |
20 |
41 |
|
24 |
Telangana |
834 |
82 |
41 |
5 |
9 |
|
25 |
Tripura |
117 |
23 |
12 |
7 |
1 |
|
26 |
Uttarakhand |
607 |
80 |
19 |
13 |
3 |
|
27 |
Uttar Pradesh |
3513 |
841 |
0 |
169 |
20 |
|
28 |
West Bengal |
1371 |
348 |
60 |
18 |
18 |
|
29 |
Andaman & Nicobar Islands |
27 |
4 |
0 |
2 |
1 |
|
30 |
Chandigarh |
43 |
2 |
1 |
1 |
2 |
|
31 |
Dadra & Nagar Haveli and Daman & Diu |
14 |
4 |
1 |
2 |
1 |
|
32 |
Delhi |
550 |
0 |
10 |
40 |
13 |
|
33 |
Jammu & Kashmir |
973 |
79 |
0 |
15 |
8 |
|
34 |
Ladakh |
33 |
7 |
0 |
2 |
0 |
|
35 |
Lakshadweep |
4 |
3 |
2 |
1 |
0 |
|
36 |
Puducherry |
39 |
4 |
0 |
4 |
2 |
|
|
All India |
31053 |
6064 |
1275 |
767 |
315 |
Note: Chandigarh has no Rural area; Delhi has no CHCs Source: Rural Health Statistics 2021-22
Availability of Doctors, Nurses & Health Workers and Other Health Professionals in PHCs & CHCs:
The MoS Health also provided the State/ UT wise details of in-positions of doctors, nurses, health workers and other health professionals as per Rural Health Statistics (RHS) 2021-2022.
As per the data, altogether 26818 Health Workers (Female)/ANM are available in rural PHCs and 21501 are available in the urban areas. Further, there are 11329 Health Assistants, 8473 Ayush doctors are available in the rural PHCs.
The data revealed that the rural PHCs have 30640 doctors, 19359 pharmacists, 14565 laboratory technicians, and 36079 nursing staff in position. On the other hand, the urban PHCs have 7315 doctors, 5029 pharmacists, 4361 laboratory technicians, and 9467 nursing staff in position.
In the case of CHCs, the rural areas have 661 Ayush specialists, 4485 Total Specialists [Surgeons, OB&GY, Physicians & Paediatricians], 17348 General Duty Medical officers, 2448 Radiographers, 7776 Pharmacists, 8207 Laboratory Technicians, and 43854 nursing staff in positions.
On the other hand, the urban CHCs have 1278 Total Specialists [Surgeons, OB&GY, Physicians & Paediatricians], 1568 GDMOs, 358 Radiographers, 840 pharmacists, 4361 Laboratory Technicians, and 6121 Nursing Staff.
State/UT wise details of availability of doctors, nurses, health workers and other health professionals and vacancies thereof, as reported by States/UTs Annexure-II
|
S. No. |
State/UT |
HEALTH WORKER [FEMALE] / ANM AT PHCs |
HEALTH ASSISTANT at PHCs |
AYUSH Doctor at PHCs |
DOCTORS at PHCs |
PHARMACISTS at PHCs |
LABORATORY TECHNICIANS at PHCs |
NURSING STAFF (STAFF NURSE) at PHCs |
|||||||||||||||||
|
Rural |
Urban |
Rural |
Rural |
Rural |
Urban |
Rural |
Urban |
Rural |
Urban |
Rural |
Urban |
||||||||||||||
|
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
In Position |
Vacant |
||
|
1 |
Andhra Pradesh |
0 |
0 |
3836 |
70 |
0 |
0 |
251 |
131 |
2048 |
158 |
484 |
63 |
1067 |
204 |
479 |
68 |
1008 |
291 |
517 |
30 |
2870 |
456 |
996 |
98 |
|
2 |
Arunachal Pradesh |
148 |
NA |
25 |
NA |
83 |
NA |
29 |
NA |
129 |
NA |
23 |
NA |
41 |
NA |
4 |
NA |
65 |
NA |
16 |
NA |
239 |
NA |
34 |
NA |
|
3 |
Assam |
1368 |
* |
304 |
6 |
112 |
139 |
270 |
63 |
1381 |
236 |
141 |
23 |
974 |
36 |
96 |
1 |
913 |
63 |
86 |
4 |
1652 |
271 |
180 |
22 |
|
4 |
Bihar |
1608 |
268 |
395 |
131 |
188 |
875 |
2497 |
524 |
1538 |
2057 |
335 |
287 |
261 |
951 |
87 |
146 |
687 |
450 |
109 |
116 |
2454 |
849 |
327 |
314 |
|
5 |
Chhattisgarh |
774 |
174 |
170 |
8 |
222 |
274 |
230 |
132 |
491 |
476 |
96 |
23 |
557 |
216 |
54 |
9 |
500 |
287 |
53 |
7 |
1545 |
431 |
147 |
36 |
|
6 |
Goa |
150 |
37 |
10 |
22 |
0 |
0 |
66 |
0 |
66 |
8 |
8 |
0 |
53 |
8 |
2 |
0 |
30 |
4 |
6 |
* |
85 |
59 |
9 |
3 |
|
7 |
Gujarat |
1037 |
538 |
2100 |
134 |
1586 |
421 |
887 |
122 |
1692 |
185 |
302 |
32 |
1324 |
194 |
305 |
21 |
1352 |
140 |
321 |
14 |
1512 |
402 |
400 |
99 |
|
8 |
Haryana |
0 |
0 |
715 |
52 |
282 |
118 |
68 |
26 |
591 |
200 |
102 |
3 |
227 |
164 |
102 |
3 |
190 |
243 |
103 |
4 |
962 |
406 |
140 |
6 |
|
9 |
Himachal Pradesh |
71 |
51 |
4 |
NA |
26 |
27 |
4 |
10 |
501 |
150 |
22 |
0 |
397 |
156 |
15 |
4 |
55 |
118 |
0 |
2 |
118 |
112 |
8 |
4 |
|
10 |
Jharkhand |
485 |
97 |
194 |
149 |
25 |
266 |
37 |
60 |
285 |
6 |
32 |
31 |
62 |
229 |
40 |
35 |
96 |
195 |
45 |
28 |
207 |
84 |
50 |
98 |
|
11 |
Karnataka |
4824 |
1383 |
1074 |
222 |
2678 |
1260 |
318 |
23 |
2078 |
414 |
413 |
49 |
1460 |
620 |
289 |
41 |
1540 |
339 |
322 |
17 |
3226 |
266 |
645 |
82 |
|
12 |
Kerala |
1741 |
211 |
448 |
23 |
NA |
NA |
NA |
NA |
1503 |
61 |
259 |
17 |
933 |
9 |
156 |
4 |
484 |
23 |
102 |
11 |
1489 |
41 |
282 |
27 |
|
13 |
Madhya Pradesh |
2552 |
126 |
898 |
* |
308 |
365 |
318 |
NA |
1631 |
315 |
271 |
35 |
958 |
308 |
53 |
50 |
621 |
645 |
40 |
66 |
1812 |
* |
383 |
* |
|
14 |
Maharashtra |
2048 |
578 |
2598 |
39 |
3269 |
479 |
91 |
63 |
3239 |
721 |
844 |
182 |
1531 |
293 |
519 |
106 |
1323 |
519 |
465 |
94 |
1310 |
623 |
1456 |
259 |
|
15 |
Manipur |
250 |
6 |
32 |
* |
40 |
12 |
72 |
6 |
308 |
35 |
17 |
0 |
131 |
3 |
9 |
1 |
76 |
14 |
4 |
* |
210 |
36 |
19 |
0 |
|
16 |
Meghalaya |
324 |
* |
64 |
* |
137 |
11 |
64 |
7 |
171 |
7 |
24 |
* |
140 |
* |
26 |
* |
148 |
* |
18 |
* |
392 |
* |
19 |
* |
|
17 |
Mizoram |
5 |
* |
17 |
* |
7 |
* |
11 |
* |
57 |
* |
10 |
* |
28 |
* |
8 |
* |
58 |
* |
11 |
* |
176 |
* |
30 |
* |
|
18 |
Nagaland |
219 |
* |
19 |
* |
33 |
* |
15 |
0 |
130 |
8 |
7 |
* |
95 |
* |
7 |
0 |
74 |
* |
8 |
0 |
200 |
* |
14 |
0 |
|
19 |
Odisha |
812 |
327 |
475 |
41 |
0 |
0 |
891 |
132 |
990 |
343 |
107 |
13 |
1148 |
183 |
102 |
16 |
350 |
21 |
94 |
10 |
546 |
1603 |
174 |
40 |
|
20 |
Punjab |
39 |
38 |
267 |
63 |
211 |
52 |
151 |
81 |
418 |
189 |
141 |
43 |
427 |
127 |
77 |
36 |
280 |
186 |
60 |
40 |
572 |
526 |
177 |
84 |
|
21 |
Rajasthan |
2400 |
415 |
690 |
143 |
1080 |
666 |
483 |
387 |
2150 |
316 |
332 |
58 |
712 |
913 |
122 |
97 |
1330 |
691 |
136 |
92 |
4097 |
754 |
518 |
68 |
|
22 |
Sikkim |
65 |
2 |
2 |
* |
27 |
0 |
5 |
0 |
38 |
1 |
3 |
* |
17 |
2 |
0 |
0 |
39 |
* |
2 |
* |
112 |
* |
17 |
* |
|
23 |
Tamil Nadu |
2475 |
237 |
1139 |
242 |
515 |
190 |
224 |
251 |
2722 |
264 |
564 |
74 |
1171 |
228 |
390 |
70 |
1013 |
409 |
410 |
52 |
4527 |
591 |
1378 |
208 |
|
24 |
Telangana |
0 |
0 |
735 |
196 |
0 |
0 |
23 |
32 |
802 |
360 |
314 |
108 |
529 |
49 |
106 |
6 |
503 |
104 |
104 |
9 |
1326 |
404 |
477 |
81 |
|
25 |
Tripura |
68 |
NA |
25 |
NA |
16 |
NA |
83 |
NA |
236 |
NA |
20 |
NA |
130 |
NA |
13 |
NA |
114 |
NA |
15 |
NA |
514 |
NA |
9 |
NA |
|
26 |
Uttarakhand |
136 |
101 |
154 |
15 |
14 |
69 |
111 |
16 |
483 |
140 |
70 |
17 |
442 |
43 |
60 |
1 |
34 |
101 |
35 |
17 |
140 |
226 |
84 |
28 |
|
27 |
Uttar Pradesh |
1966 |
1291 |
2142 |
120 |
289 |
1269 |
478 |
737 |
2890 |
1558 |
462 |
134 |
2710 |
557 |
490 |
63 |
976 |
1044 |
457 |
91 |
1247 |
2427 |
827 |
176 |
|
28 |
West Bengal |
0 |
0 |
608 |
1481 |
35 |
50 |
263 |
105 |
975 |
563 |
605 |
365 |
796 |
118 |
330 |
118 |
235 |
426 |
359 |
143 |
1685 |
72 |
466 |
459 |
|
29 |
Andaman & Nicobar Islands |
40 |
6 |
16 |
0 |
3 |
2 |
20 |
5 |
50 |
3 |
10 |
0 |
17 |
4 |
5 |
0 |
20 |
0 |
4 |
1 |
95 |
1 |
5 |
0 |
|
30 |
Chandigarh |
N App |
N App |
115 |
* |
N App |
N App |
N App |
N App |
N App |
N App |
67 |
* |
N App |
N App |
75 |
* |
N App |
N App |
18 |
* |
N App |
N App |
10 |
3 |
|
31 |
Dadra & Nagar Haveli and Daman & Diu |
10 |
0 |
25 |
0 |
2 |
0 |
15 |
0 |
16 |
0 |
2 |
0 |
15 |
0 |
2 |
0 |
17 |
0 |
2 |
0 |
49 |
0 |
6 |
0 |
|
32 |
Delhi |
22 |
3 |
1915 |
57 |
1 |
1 |
1 |
0 |
16 |
3 |
1064 |
82 |
3 |
1 |
868 |
97 |
6 |
1 |
362 |
16 |
6 |
0 |
N App |
N App |
|
33 |
Jammu & Kashmir |
1057 |
72 |
206 |
14 |
102 |
34 |
443 |
0 |
904 |
620 |
138 |
41 |
932 |
148 |
119 |
15 |
393 |
74 |
63 |
5 |
568 |
135 |
110 |
8 |
|
34 |
Ladakh |
40 |
1 |
0 |
0 |
0 |
0 |
26 |
4 |
54 |
54 |
1 |
0 |
39 |
2 |
0 |
0 |
8 |
3 |
0 |
0 |
11 |
1 |
0 |
0 |
|
35 |
Lakshadweep |
17 |
1 |
N App |
N App |
0 |
0 |
4 |
0 |
12 |
0 |
N App |
N App |
6 |
0 |
N App |
N App |
6 |
0 |
N App |
N App |
11 |
0 |
N App |
N App |
|
36 |
Puducherry |
67 |
0 |
84 |
0 |
38 |
0 |
24 |
0 |
45 |
0 |
25 |
0 |
26 |
* |
19 |
* |
21 |
3 |
14 |
1 |
114 |
* |
70 |
0 |
|
|
All India/ Total |
26818 |
5963 |
21501 |
3228 |
11329 |
6580 |
8473 |
2917 |
30640 |
9451 |
7315 |
1680 |
19359 |
5766 |
5029 |
1008 |
14565 |
6394 |
4361 |
870 |
36079 |
10776 |
9467 |
2203 |
Notes: NA – Not Available N App – Not Applicable *: Surplus. All India figures for Vacancy are the totals of State-wise Vacancy ignoring surplus in some States / UTs Source: Rural Health Statistics 2021-22 (as on 31st March, 2022)
Vacant Positions:
In the PHCs, 5863 Health Workers (Female)/ANM are vacant in rural areas and 3228 are vacant in urban areas. Further, there are 6580 positions of Health Assistants and 2917 posts of Ayush doctors are vacant in rural areas.
Further the data revealed that the rural PHCs have 9451 vacant positions of doctors, 5766 posts of pharmacists, 6394 laboratory technicians, and 10776 vacant nursing staff. On the other hand, the urban PHCs have 1680 doctors, 1008 pharmacists, 870 laboratory technicians, and 2203 nursing staff posts vacant.
In the case of CHCs, the rural areas have 605 Ayush specialists, 9343 Total Specialists [Surgeons, OB&GY, Physicians & Paediatricians], 5159 General Duty Medical officers, 1628 Radiographers, 1723 Pharmacists, 1752 Laboratory Technicians, and 12174 nursing staff posts vacant.
On the other hand, the urban CHCs have 764 Total Specialists [Surgeons, OB&GY, Physicians & Paediatricians], 528 GDMOs, 164 Radiographers, 179 pharmacists, 870 Laboratory Technicians, and 1433 Nursing Staff posts vacant.
State/UT wise details of availability of doctors, nurses, health workers and other health professionals and vacancies thereof, as reported by States/UTs Annexure-II (Contd.)
|
S. No. |
State/UT |
AYUSH Specialist at CHCs |
Total Specialists [Surgeons, OB&GY, Physicians & Paediatricians] at CHCs |
General Duty Medical Officers (GDMOs) – Allopathic at CHCs |
RADIOGRAPHERS at CHCs |
PHARMACISTS at CHCs |
LABORATORY TECHNICIANS at CHCs |
NURSING STAFF at CHCs |
|||||||||||||||||||
|
Rural |
Rural |
Urban |
Rural |
Urban |
Rural |
Urban |
Rural |
Urban |
Rural |
Urban |
Rural |
Urban |
|||||||||||||||
|
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
In Position |
Vacan t |
||
|
1 |
Andhra Pradesh |
10 |
14 |
264 |
144 |
114 |
48 |
165 |
65 |
46 |
18 |
47 |
54 |
26 |
16 |
149 |
42 |
58 |
18 |
189 |
42 |
517 |
30 |
1079 |
225 |
422 |
99 |
|
2 |
Arunachal Pradesh |
5 |
NA |
11 |
NA |
N App |
N App |
113 |
NA |
N App |
N App |
18 |
NA |
N App |
N App |
51 |
NA |
N App |
N App |
81 |
NA |
16 |
NA |
453 |
NA |
N App |
N App |
|
3 |
Assam |
8 |
14 |
179 |
88 |
60 |
* |
622 |
52 |
109 |
* |
93 |
12 |
28 |
0 |
389 |
* |
64 |
* |
389 |
* |
86 |
4 |
1911 |
* |
411 |
* |
|
4 |
Bihar |
59 |
87 |
322 |
959 |
64 |
109 |
931 |
676 |
68 |
60 |
29 |
146 |
4 |
24 |
163 |
202 |
27 |
31 |
221 |
248 |
109 |
116 |
2502 |
2418 |
371 |
330 |
|
5 |
Chhattisgarh |
18 |
47 |
66 |
550 |
14 |
16 |
704 |
140 |
9 |
12 |
140 |
42 |
2 |
0 |
227 |
111 |
5 |
1 |
428 |
42 |
53 |
7 |
1599 |
658 |
45 |
4 |
|
6 |
Goa |
15 |
0 |
2 |
20 |
N App |
N App |
38 |
6 |
N App |
N App |
9 |
2 |
N App |
N App |
29 |
2 |
N App |
N App |
16 |
* |
6 |
* |
82 |
13 |
N App |
N App |
|
7 |
Gujarat |
0 |
0 |
127 |
284 |
98 |
7 |
901 |
162 |
7 |
0 |
72 |
41 |
7 |
11 |
307 |
54 |
20 |
0 |
330 |
39 |
321 |
14 |
2389 |
162 |
77 |
23 |
|
8 |
Haryana |
10 |
9 |
33 |
103 |
3 |
5 |
506 |
315 |
8 |
0 |
27 |
89 |
2 |
0 |
171 |
102 |
4 |
0 |
219 |
134 |
103 |
4 |
1300 |
595 |
10 |
2 |
|
9 |
Himachal Pradesh |
0 |
0 |
18 |
NA |
2 |
NA |
265 |
93 |
19 |
2 |
36 |
19 |
2 |
0 |
121 |
62 |
12 |
* |
61 |
72 |
0 |
2 |
329 |
106 |
35 |
1 |
|
10 |
Jharkhand |
114 |
57 |
207 |
477 |
5 |
16 |
710 |
* |
3 |
4 |
120 |
51 |
0 |
0 |
167 |
4 |
3 |
10 |
281 |
10 |
45 |
28 |
1165 |
* |
4 |
24 |
|
11 |
Karnataka |
12 |
8 |
263 |
198 |
70 |
32 |
167 |
40 |
23 |
15 |
114 |
28 |
21 |
0 |
181 |
126 |
37 |
10 |
283 |
27 |
322 |
17 |
1632 |
247 |
315 |
73 |
|
12 |
Kerala |
NA |
NA |
48 |
2 |
4 |
1 |
456 |
117 |
68 |
1 |
13 |
4 |
3 |
0 |
256 |
1 |
29 |
1 |
232 |
* |
102 |
11 |
1451 |
186 |
159 |
10 |
|
13 |
Madhya Pradesh |
0 |
0 |
66 |
1127 |
62 |
34 |
824 |
166 |
32 |
112 |
195 |
137 |
6 |
18 |
467 |
* |
17 |
25 |
530 |
* |
40 |
66 |
2837 |
509 |
115 |
148 |
|
14 |
Maharashtra |
53 |
6 |
313 |
139 |
245 |
102 |
458 |
110 |
369 |
88 |
98 |
39 |
53 |
12 |
303 |
36 |
233 |
8 |
256 |
49 |
465 |
94 |
1862 |
322 |
1801 |
106 |
|
15 |
Manipur |
4 |
1 |
18 |
14 |
8 |
10 |
125 |
35 |
11 |
3 |
7 |
3 |
6 |
2 |
32 |
* |
20 |
* |
37 |
4 |
4 |
* |
195 |
22 |
119 |
18 |
|
16 |
Meghalaya |
0 |
0 |
5 |
0 |
N App |
N App |
100 |
* |
N App |
N App |
21 |
* |
N App |
N App |
43 |
* |
N App |
N App |
50 |
* |
18 |
* |
407 |
* |
N App |
N App |
|
17 |
Mizoram |
1 |
* |
0 |
0 |
N App |
N App |
11 |
* |
N App |
N App |
4 |
* |
N App |
N App |
5 |
* |
N App |
N App |
15 |
* |
11 |
* |
37 |
* |
N App |
N App |
|
18 |
Nagaland |
0 |
0 |
9 |
NA |
N App |
N App |
47 |
15 |
N App |
N App |
2 |
0 |
N App |
N App |
21 |
2 |
N App |
N App |
51 |
* |
8 |
0 |
223 |
* |
N App |
N App |
|
19 |
Odisha |
0 |
0 |
306 |
1206 |
11 |
27 |
1430 |
950 |
36 |
8 |
70 |
107 |
1 |
1 |
599 |
165 |
23 |
0 |
550 |
194 |
94 |
10 |
2096 |
1422 |
50 |
42 |
|
20 |
Punjab |
8 |
8 |
151 |
426 |
19 |
19 |
459 |
14 |
32 |
11 |
167 |
13 |
1 |
4 |
304 |
72 |
5 |
8 |
326 |
82 |
60 |
40 |
1282 |
537 |
24 |
30 |
|
21 |
Rajasthan |
44 |
34 |
525 |
1030 |
162 |
79 |
1730 |
228 |
236 |
48 |
356 |
344 |
64 |
32 |
486 |
249 |
70 |
14 |
819 |
346 |
136 |
92 |
5186 |
1321 |
810 |
148 |
|
22 |
Sikkim |
0 |
0 |
0 |
0 |
N App |
N App |
4 |
0 |
N App |
N App |
4 |
0 |
N App |
N App |
5 |
0 |
N App |
N App |
8 |
0 |
2 |
* |
33 |
0 |
N App |
N App |
|
23 |
Tamil Nadu |
68 |
14 |
249 |
88 |
29 |
26 |
2100 |
98 |
32 |
26 |
220 |
54 |
1 |
4 |
411 |
67 |
19 |
2 |
557 |
38 |
410 |
52 |
3384 |
350 |
209 |
56 |
|
24 |
Telangana |
8 |
3 |
98 |
14 |
156 |
109 |
64 |
20 |
87 |
61 |
24 |
4 |
29 |
23 |
24 |
4 |
56 |
14 |
23 |
0 |
104 |
9 |
257 |
107 |
428 |
176 |
|
25 |
Tripura |
0 |
NA |
3 |
NA |
0 |
NA |
74 |
NA |
11 |
NA |
12 |
NA |
2 |
NA |
33 |
NA |
2 |
NA |
36 |
NA |
15 |
NA |
169 |
NA |
19 |
NA |
|
26 |
Uttarakhand |
3 |
12 |
36 |
126 |
21 |
72 |
212 |
33 |
137 |
0 |
17 |
17 |
11 |
9 |
68 |
7 |
39 |
10 |
47 |
25 |
35 |
17 |
211 |
141 |
176 |
74 |
|
27 |
Uttar Pradesh |
221 |
291 |
918 |
2028 |
35 |
23 |
2311 |
1097 |
10 |
0 |
179 |
329 |
1 |
1 |
1929 |
260 |
10 |
0 |
1208 |
251 |
457 |
91 |
5341 |
2669 |
83 |
17 |
|
28 |
West Bengal |
0 |
0 |
97 |
192 |
N App |
N App |
1311 |
591 |
N App |
N App |
129 |
62 |
N App |
N App |
581 |
112 |
N App |
N App |
687 |
117 |
359 |
143 |
3655 |
* |
N App |
N App |
|
29 |
Andaman & Nicobar Islands |
0 |
0 |
4 |
12 |
N App |
N App |
16 |
2 |
N App |
N App |
4 |
0 |
N App |
N App |
13 |
7 |
N App |
N App |
4 |
3 |
4 |
1 |
56 |
6 |
N App |
N App |
|
30 |
Chandigarh |
N App |
N App |
N App |
N App |
15 |
* |
N App |
N App |
21 |
* |
N App |
N App |
13 |
* |
N App |
N App |
8 |
* |
N App |
N App |
18 |
* |
N App |
N App |
67 |
* |
|
31 |
Dadra & Nagar Haveli and Daman & Diu |
0 |
0 |
0 |
0 |
0 |
0 |
11 |
0 |
1 |
0 |
0 |
0 |
0 |
0 |
11 |
0 |
1 |
0 |
7 |
0 |
2 |
0 |
40 |
0 |
2 |
0 |
|
32 |
Delhi |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
N App |
362 |
16 |
N App |
N App |
N App |
N App |
|
33 |
Jammu & Kashmir |
0 |
0 |
127 |
101 |
79 |
29 |
423 |
99 |
186 |
59 |
204 |
30 |
74 |
7 |
197 |
32 |
75 |
27 |
234 |
26 |
63 |
5 |
581 |
158 |
357 |
52 |
|
34 |
Ladakh |
0 |
0 |
12 |
15 |
N App |
N App |
27 |
35 |
N App |
N App |
8 |
1 |
N App |
N App |
19 |
2 |
N App |
N App |
16 |
3 |
0 |
0 |
41 |
0 |
N App |
N App |
|
35 |
Lakshadweep |
0 |
0 |
8 |
0 |
N App |
N App |
13 |
0 |
N App |
N App |
6 |
0 |
N App |
N App |
7 |
2 |
N App |
N App |
9 |
0 |
N App |
N App |
35 |
0 |
N App |
N App |
|
36 |
Puducherry |
0 |
0 |
0 |
0 |
2 |
0 |
20 |
0 |
7 |
0 |
3 |
0 |
1 |
0 |
7 |
* |
3 |
0 |
7 |
* |
14 |
1 |
34 |
0 |
12 |
0 |
|
|
All India/ Total |
661 |
605 |
4485 |
9343 |
1278 |
764 |
17348 |
5159 |
1568 |
528 |
2448 |
1628 |
358 |
164 |
7776 |
1723 |
840 |
179 |
8207 |
1752 |
4361 |
870 |
43854 |
12174 |
6121 |
1433 |
Notes: NA – Not Available N App – Not Applicable *: Surplus. All India figures for Vacancy are the totals of State-wise Vacancy ignoring surplus in some States / UTs Source: Rural Health Statistics 2021-22 (as on 31st March 2022)
“Public Health and Hospitals is a State Subject and all the administrative and personnel matters, including support for outsourcing or engagement of doctors and other health human resources lies with the respective State Government/UT Administration. Further, under National Health Mission (NHM), Government of India provides financial and technical support to States/UTs to strengthen their healthcare systems,” informed the MoS Health.
As per the Minister, the Government of India has taken the following initiatives in the form of incentives and honorarium to the medical professionals for encouraging better service delivery in rural and remote areas in the country,
Hard area allowance to specialist doctors for serving in rural and remote areas and for their residential quarters so that they find it attractive to serve in public health facilities in such areas.
Honorarium to Gynecologists/ Emergency Obstetric Care (EmoC) trained, Pediatricians & Anesthetist/ Life Saving Anaesthesia Skills (LSAS) trained doctors to increase availability of specialists for conducting Cesarean sections in rural & remote area.
Incentives like special incentives for doctors, incentive for ANM for ensuring timely ANC checkup and recording, incentives for conducting Adolescent Reproductive and Sexual Health activities.
States are also allowed to offer negotiable salary to attract specialist including flexibility in strategies such as “You Quote We Pay”.
Non-Monetary incentives such as preferential admission in post graduate courses for staff serving in difficult areas and improving accommodation arrangement in rural areas have also been introduced under NHM.
Multi-skilling of doctors is supported under NHM to overcome the shortage of specialists. Skill upgradation of existing HR is another major strategy under NRHM for achieving improvement in health outcomes.
Also Read: 80% Shortfall of Specialist Doctors in CHCs: Health Ministry Report
Powered by WPeMatico

New Delhi: The Indian Council of Medical Research (ICMR), under the Department of Health Research, has recently published Standard Treatment Workflows (STWs). These workflows outline standardized protocols and drug treatments for managing both common and serious diseases encountered by healthcare providers at all levels, the Minister of State Health and Family Welfare Shri Prataprao Jadhav informed Lok Sabha.
The MoS Jadhav stated,”In accordance with Rule 9(iii) of the Clinical Establishments (Central Government) Rules, 2012, every clinical establishment must adhere to the Standard Treatment Guidelines (STGs) as established and disseminated by the Central Government or the State Government, as applicable, periodically for the purposes of registration and ongoing compliance”.
The Minister said this in a written statement to the parliament when asked for the details of whether the Government has issued Standard Treatment Guidelines (STGs) regarding prescriptions issued by doctors, if so, the details thereof.
A series of questions were raised by Parliament member Bhartruhari Mahtab who sought to know from the minister whether as per the study by Indian Journal of Medical Research (IJMR) nearly 50 percent of Government doctors prescriptions deviate from guidelines and if so, details thereof; and whether the Government is considering to issue revised guidelines in consultation with the doctors. if so, details thereof?
In response to these questions, MoS Health said, “Indian Council of Medical Research (ICMR), under the Department of Health Research has recently developed and released the Standard Treatment Workflows (STWs) encompassing standardized protocols and drug treatment prescribed in the management of common and serious diseases encountered by the treating doctors across all levels of healthcare.”
The STWs provide the relevant key indicative actions and treatment for various disease conditions. These have to be utilized at various levels of healthcare starting from primary to tertiary level care and are made available by the Government of India and recommended to be adopted and followed by all healthcare providers across the country uniformly. The STWs in 4 volumes cover a wide range of 157 Medical/surgical diseases/conditions across 28 medical specialties. The STWs have been prepared by national subject experts across the country, added the Minister.
Further, the minister stated, “The study in reference, titled ‘Evaluation of prescriptions from tertiary care hospitals across India for deviations from treatment guidelines & their potential consequences’, published in the Indian Journal of Medical Research (IJMR), has analysed the outpatient prescriptions by physicians of various specialties in tertiary care, teaching government and private hospitals. It is pertinent to note that the study has some limitations in the form, sample representation, single-time point data collection, potential bias in data collection, lack of longitudinal follow-up, etc. Thus, the study is inadequate to be generalized with respect to interpreted results.”
Powered by WPeMatico
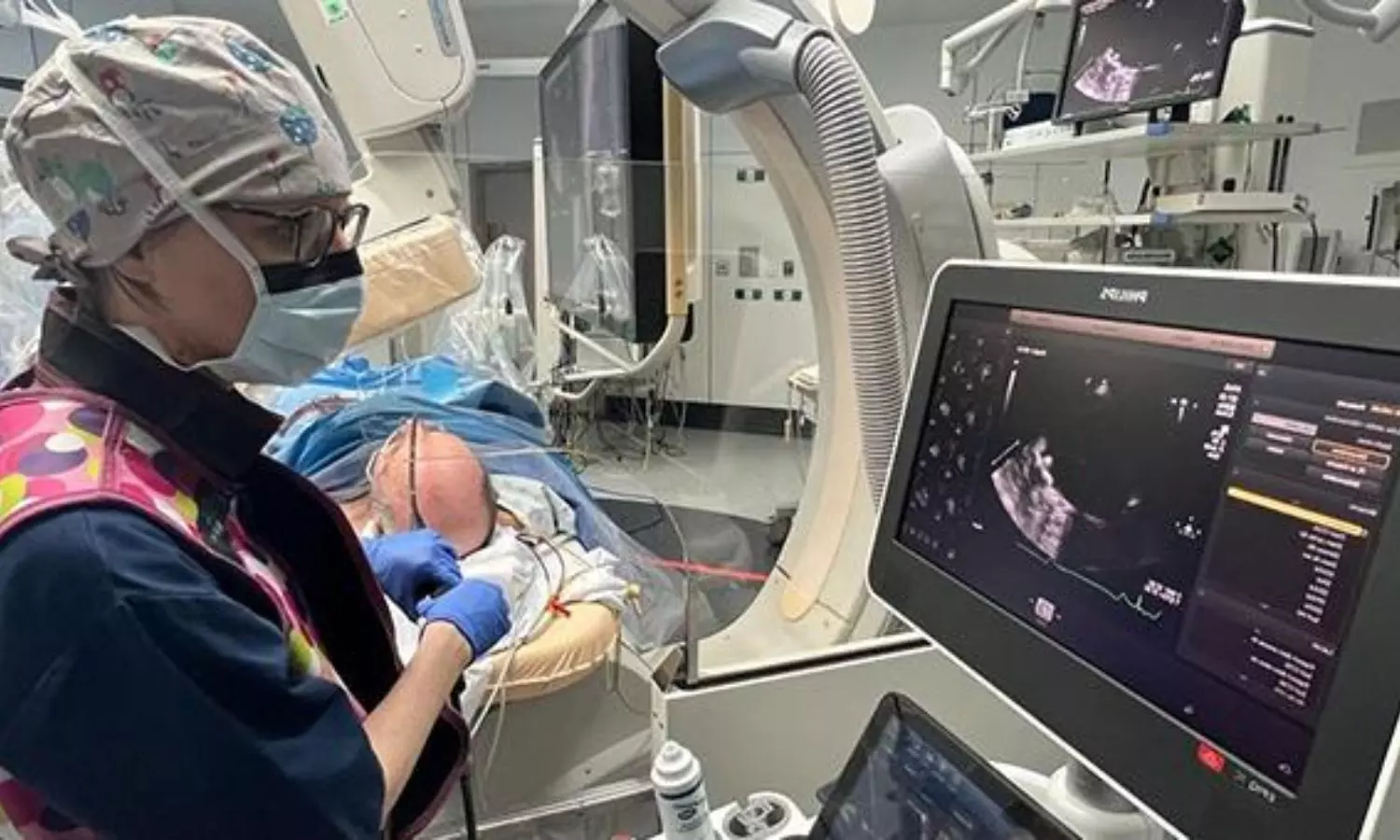
Transesophageal echocardiography (TEE) is extensively utilized in cardiac surgery to provide real-time, high-resolution images of the heart and its surrounding structures, contributing significantly to surgical decision-making, procedural monitoring, and postoperative outcome assessment. Recent study investigated factors predictive of difficult transesophageal echocardiography (TEE) probe insertion in adult cardiac surgery patients. The observational study involved 119 adult patients undergoing cardiac surgery, analyzing demographic variables (age, gender, BMI) and airway factors (modified Mallampati classification, modified Cormack-Lehane grading, and thyromental distance). The difficulty of TEE probe insertion was categorized into three grades, and various maneuvers were assessed for difficult insertions.
Results and Key Findings
Results showed that 30.3% of insertions were difficult, and male gender, BMI ≥30 kg/m2, Mallampati class III-IV, Cormack-Lehane grade IIb-IV, and thyromental distance <6.5 cm were significantly associated with difficult insertion. Jaw thrust was the most effective maneuver for difficult cases, used in 58.3% of instances. The study highlighted the potential complications associated with difficult TEE probe insertion, such as oropharyngeal injuries and esophageal perforation, particularly with larger 3D TEE probes. The findings emphasized the importance of identifying predictive factors to anticipate challenges and reduce complications.
Patient Characteristics and Airway Factors
The study involved ethical approval and excluded patients with contraindications to TEE probe placement. The age of participants ranged from 18 to 75 years, with a higher proportion of males. The BMI distribution showed a significant portion of overweight and obese patients. Airway characteristics, including Mallampati scores and Cormack-Lehane grading, indicated potential difficulties with TEE probe insertion. While the majority of insertions were performed without difficulty, 30.3% required intervention, with jaw thrust being the most commonly used and effective technique.
Statistical Associations
The study found statistical associations between demographic and airway factors and difficult TEE probe insertion, with Mallampati class III-IV showing the strongest association. Men, individuals with high BMI, and unfavorable airway characteristics were also significantly associated with difficulty. The use of video laryngoscopy was not required in any case, suggesting that simpler techniques were sufficient. The study provided valuable insights into the predictive factors associated with difficult TEE probe insertion, highlighting the importance of comprehensive preoperative airway assessment and the value of simple, effective maneuvers in managing insertion difficulties. The findings emphasized the need for further research to validate the results in larger, multi-center studies and explore additional predictive tools to enhance patient safety during TEE probe insertion.
Key Points
– The study aimed to identify factors predictive of difficult transesophageal echocardiography (TEE) probe insertion in adult cardiac surgery patients. It involved 119 adult patients undergoing cardiac surgery and analyzed demographic variables (age, gender, BMI) and airway factors (modified Mallampati classification, modified Cormack-Lehane grading, and thyromental distance). – Results indicated that 30.3% of insertions were difficult, with male gender, BMI ≥30 kg/m2, Mallampati class III-IV, Cormack-Lehane grade IIb-IV, and thyromental distance <6.5 cm being significantly associated with difficult insertion. Jaw thrust was the most effective maneuver for difficult cases, used in 58.3% of instances. – The study highlighted potential complications associated with difficult TEE probe insertion, such as oropharyngeal injuries and esophageal perforation, particularly with larger 3D TEE probes. It stressed the importance of identifying predictive factors to anticipate challenges and reduce complications. – Statistical associations were found between demographic and airway factors and difficult TEE probe insertion, with Mallampati class III-IV showing the strongest association. Men, individuals with high BMI, and unfavorable airway characteristics were also significantly associated with difficulty. Video laryngoscopy was not required in any case, suggesting that simpler techniques were sufficient. – The study emphasized the importance of comprehensive preoperative airway assessment and the value of simple, effective maneuvers in managing insertion difficulties. It also called for further research to validate the results in larger, multi-center studies and explore additional predictive tools to enhance patient safety during TEE probe insertion.
Reference –
Hasnain S, Shenava A, Garg I (July 10, 2024) A Study of Factors Predicting Difficulties in Transesophageal Echocardiography (TEE) Probe Insertion in Adult Patients Undergoing Cardiac Surgery. Cureus 16(7): e64256. DOI 10.7759/cureus.64256.
Powered by WPeMatico
Researchers from the University of Adelaide could be closer to discovering a better way to use metformin, a common type 2 diabetes medication.
Metformin, which has been a cornerstone in diabetes treatment since the 1960s, is typically taken with meals to reduce gastrointestinal side effects but new research is suggesting patients could see improved results if it’s taken before meals.
Dr Cong Xie postdoctoral research fellow in the Centre of Research Excellence in Translating Nutritional Science to Good Health, at Adelaide Medical School, worked with Associate Professor Tongzhi Wu and a team which studied the gastrointestinal effects of the drug on 16 people living with type 2 diabetes who were already using it to treat the condition.
Their findings were published in the journal Diabetologia and are now being used in e-learning by the European Association for the Study of Diabetes (one of the largest international platforms for diabetes research and clinical practice).
“Our results demonstrate administering metformin 30 to 60 minutes before a meal reduces plasma glucose levels while increasing the secretion of the incretin hormone glucagon-like peptide 1 (GLP-1) and insulin levels,” Dr Xie said.
“GLP-1 is a hormone secreted from the gut, which exhibits several actions, including the suppression of appetite, stimulation of insulin, slowing of gastric emptying and the subsequent glucose absorption in the intestine, all of which are beneficial for the control of blood sugar and body weight.
“A number of GLP-1-based drugs are now used clinically for the management of obesity and type 2 diabetes; these drugs also reduce the risk of cardiovascular disease.”
Dr Xie said the plasma GLP-1 levels increased only when metformin was given before the subjects were given a glucose infusion and not at the same time.
“This suggests the levels are affected by changes in the glucose-gut interaction,” he said.
Associate Professor Wu said the study found there was no real difference to the nausea scores of patients between the administration times.
“The findings of our study suggest that the empirical recommendation for ingestion of metformin with meals may have compromised its efficacy to improve blood glucose control after meals,” he said.
“Modification of the timing of metformin ingestion in relation to meals could be a cost-effective approach to improve glycaemic control in people living with type 2 diabetes.”
“We are now planning to extend this research in a real-world setting to examine whether administration of metformin before meals will lead to better blood glucose control in people with type 2 diabetes in the long term.”
Reference:
Xie, C., Iroga, P., Bound, M.J. et al. Impact of the timing of metformin administration on glycaemic and glucagon-like peptide-1 responses to intraduodenal glucose infusion in type 2 diabetes: a double-blind, randomised, placebo-controlled, crossover study. Diabetologia 67, 1260–1270 (2024). https://doi.org/10.1007/s00125-024-06131-6.
Powered by WPeMatico
