Research shows that smartwatch and clinical testing measures differ
Powered by WPeMatico
Powered by WPeMatico

New Delhi: Emphasizing the urgent need for measures to safeguard the security of medical professionals across the country, the National Task Force (NTF), established by the Supreme Court in response to the brutal rape and murder of a postgraduate medico in Kolkata, held its inaugural meeting on August 27.
The meeting was attended by all members of the NTF, which is tasked with making recommendations to enhance the safety and security of medical professionals in their workplaces, according to official sources.
National Task Force member Dr Saumitra Rawat earlier told ANI that the top court has asked the task force to file an interim report within three weeks and the final report within two months.
According to an ANI report, Dr Rawat, who is also the Chairman and Head of the Institute of Surgical Gastroenterology, SGRH, further explained the areas that will be focussed in the report regarding the safety of doctors and nurses and said, “We are expected to work in two different areas, it has been told to us by the CJI – the first issue is preventing violence against medical professional, second is to draft a national protocol for dignified and safe working for the doctors, nurses and all the paramedical staffs.”
“So we, or everybody in the committee, we will work together, and we will come up with the guidelines,” he added.
According to an office memorandum issued by the Union Health Ministry, the 14-member NTF has been constituted with the composition of Ex-officio Members and experts of the medical profession, Cabinet Secretary, Government of India – Chairperson, Home Secretary, Government of India, Secretary, Ministry of Health and Family Welfare – Member Secretary Government of India, Chairperson, National Medical Commission, President, National Board of Examinations, Surgeon Vice Admiral Arti Sarin, AVSM, VSM, Director General Medical Services (Navy), Dr D Nageshwar Reddy, Chairman and Managing Director, Asian Institute of Gastroenterology and AIG Hospitals, Hyderabad, Dr M Srinivas, Director, All India Institute of Medical Sciences, (AIIMS), Delhi, Dr Pratima Murthy, Director, National Institute of Mental Health and Neurosciences (NIMHANS), Bengaluru, Dr Goverdhan Dutt Puri, Executive Director, All India Institute of Medical Sciences, Jodhpur Dr Saumitra Rawat, Chairperson, Institute of Surgical Gastroenterology, GI and HPB Onco-Surgery and Liver Transplantation and Member, Board of Management, Sir Ganga Ram Hospital, New Delhi, Professor Anita Saxena, Vice-Chancellor, Pandit BD Sharma Medical University, Rohtak, Formerly Dean of Academics, Chief-Cardiothoracic Centre and Head Cardiology Department at All India Institute of Medical Sciences (AIIMS), Delhi, Dr Pallavi Saple, Dean, Grant Medical College and Sir JJ Group of Hospitals, Mumbai and Dr Padma Srivastava, formerly Professor at the Department of Neurology, news agency ANI reported.
Powered by WPeMatico

Amravati: The life of 22-year-old chemical engineer C. Harika, tragically lost in the recent industrial disaster in Anakapalli district, might have been saved if her employer had granted her an additional day of leave.
Harika, a young engineer from Kakinada, had recently returned home to celebrate Raksha Bandhan with her family. She sought an extra day off to attend a competitive examination on Wednesday. However, Escientia Advanced Sciences Pvt. Ltd. that manufactures intermediate chemicals and active pharmaceutical ingredients (API), denied her request for leave, local reports said.
As fate would have it, she came back to work only to become a victim of the powerful vapour cloud explosion at 2.20 pm on August 21 in the pharma unit in Atchutapuram.
She was one of the 17 people who perished, leaving her family in deep sorrow.
According to PTI, Harika had lost her father some years ago, and it’s reported that her older brother had abandoned the family.
Despite these odds, she went on to study engineering, living with her mother and paternal grandmother.
Family members, neighbours and locals mourned her loss and were inconsolable on receiving her body on Thursday, following a post-mortem examination.
Meanwhile, the relatives of other deceased victims and injured workers vented their anger against the tight-lipped management of the company for not notifying them about the disaster.
“How can they not inform us? Did they hire these employees without interviews and taking their certificates? Where did the managing director go? Didn’t they take our (employees’) documents such as Aadhaar while joining?” thundered a frustrated woman while talking to a regional language news channel.
She questioned whether the management did not note the addresses of the employees while recruiting them and if it didn’t know how many employees were on shift and how many of them went missing.
Amid the many workers present at the plant during the disaster were a few lucky ones who managed to escape the horrifying accident, and K Satyanarayana (30) from Eluru is one of them.
“I ate lunch and sat in the quality control (QC) department on the first floor. Then we heard a big sound as if something collapsed. Immediately, I went down and saw several people injured. I saw one man with severed hands,” Satyanarayana told PTI.
Besides seeing several workers with bleeding injuries, he also noticed that all the equipment in the production laboratory located on the ground floor had fallen down and that the explosion had blown the second floor slab away.
Eager to escape, Satyanarayana, along with 11 others, tried to flee through the emergency exits but all of them were engulfed in fumes, prompting them to break a window on the third floor and raise an alarm to rescue them.
“After two hours, ladder vehicles were brought and all 11 of us were rescued around 4.30 pm. I am a QC executive, I do analysis. I joined the company only two months ago,” he said.
According to Satyanarayana, 400 people work in three shifts to run the unit 24×7.
The management of the plant located on a 40-acre campus in the Andhra Pradesh Industrial Infrastructure Corporation’s multi-product SEZ at the Atchutapuram cluster is believed to be based in the US.
State Home Minister Vangalapudi Anitha complained that the management had ignored her calls when she went to take stock of the inferno.
Escientia Advanced Sciences commenced production in April 2019 with an investment of Rs 200 crore.
Powered by WPeMatico

Gurugram: Gurugram is set to receive a boost to its healthcare infrastructure with the nearing completion of the Sheetla Mata Hospital. The advanced facility, which is nearing the final stages of construction, is expected to be officially handed over by early 2025.
The structural work for the Sheetla Mata Hospital and Medical College building in Kherki Majra village, near the Dwarka Expressway, is scheduled to be completed by September this year. The building will then be handed over to either the Health Department or the Medical Education Department in March of next year.
GMDA officials reported that the finishing work on the building is also underway and is expected to be completed by March of next year. A senior official from the Health Department noted that the hospital is expected to be managed by either the Health Department or the State Medical Education Department, and a proposal for this arrangement has already been submitted to the government.
The Sheetla Mata Hospital and Medical College building in Kherki Majra village is expected to have its structural work completed by September 2024. According to officials from the Gurugram Metropolitan Development Authority (GMDA), the entire complex is expected to be handed over to either the Health or Medical Education Department by March 2025. The finishing touches are currently in progress and are also set to be completed by the March deadline. This new addition is anticipated to improve healthcare accessibility and outcomes for the city’s residents.
Also Read: Haryana: PHCs to be Upgraded, New CHCs to be set up
As per The Hindustan Times report, Vikas Malik, the GMDA executive engineer is overseeing the project. He noted that the major blocks of the hospital and medical college have been completed. “We have also begun the finishing work on the completed sections, and the entire complex is set to be finished by March next year. We will then hand over the complex to the authorities,” Malik added.
The hospital complex will span 30.75 acres with a built-up area of 125,000 square feet. The project will be developed for Rs 541 crore and it will also feature approximately 900 beds across 10 blocks. These blocks will include a main hospital building, a trauma center, an academic block, hostels for undergraduate students, interns, and residents, a nurse hostel, a shopping complex, and various other facilities. The project was initially announced in 2018, and the foundation stone was laid by Prime Minister Narendra Modi in September 2019.
The development of the Sheetla Mata Hospital is part of a broader initiative by local authorities to enhance healthcare services in Gurugram. A senior health department official has spoken on condition of anonymity. The official has indicated that the hospital will likely be operated by either the State Health Department or the State Medical Education Department. “An earlier plan to manage the hospital through a public-private partnership has been abandoned. The hospital is now expected to be run by state government agencies to offer affordable healthcare to the residents of Gurugram and surrounding areas,” the official added.
Also Read: Paras Healthcare lays foundation stone of 300-bed Hospital in Gurugram
Powered by WPeMatico

UK: In recent findings, glycated hemoglobin (HbA1c) has been identified as a critical marker for predicting disease severity in patients with non-alcoholic fatty liver disease (NAFLD). This revelation underscores HbA1c’s pivotal role in managing and assessing NAFLD, surpassing traditional measures such as Body Mass Index (BMI) in forecasting disease progression.
“HbA1c provides more precise insights into NAFLD severity than BMI,” the researchers wrote in their study published in Diabetes Research and Clinical Practice. “Incorporating HbA1c assessments into the comprehensive evaluation of NAFLD patients is essential, as it, along with age, helps pinpoint those at the highest risk of advanced disease.”
NAFLD, a condition characterized by excess fat accumulation in the liver independent of alcohol consumption, affects a significant portion of the global population and is often linked with metabolic disorders such as diabetes and obesity. Traditionally, BMI has been used as a primary indicator of NAFLD severity, but emerging research highlights HbA1c as a more robust predictor of disease advancement. Considering this, Santo Colosimo, Oxford University Hospitals NHS Foundation Trust, Oxford, UK, and colleagues aimed to define the relationship between HbA1c and NAFLD severity in patients with and without type 2 diabetes (T2D).
For this purpose, the researchers collected data from 857 patients with liver biopsy-confirmed NAFLD, employing generalized-linear models and binomial regression analysis to explore the relationships between histological NAFLD severity, age, HbA1c, and BMI. Additionally, paired biopsies from 421 patients involved in interventional studies were analyzed to evaluate the effects of weight changes, HbA1c levels, and active versus placebo treatments on improvements in steatosis, non-alcoholic steatohepatitis (NASH), and fibrosis.
The following were the key findings of the study:
The team concluded HbA1c is “extremely informative” for predicting NAFLD severity and offers greater insight into disease status than BMI. Specifically, a one percent-point change in HbA1c carries the same risk to liver health as an 8 kg change in body weight.
Reference:
Colosimo S, Miller H, Koutoukidis DA, Marjot T, Tan GD, Harman DJ, Aithal GP, Manousou P, Forlano R, Parker R, Sheridan DA, Newsome PN, Alazawi W, Cobbold JF, Tomlinson JW. Glycated hemoglobin is a major predictor of disease severity in patients with NAFLD. Diabetes Res Clin Pract. 2024 Aug 13:111820. doi: 10.1016/j.diabres.2024.111820. Epub ahead of print. PMID: 39147101.
Powered by WPeMatico
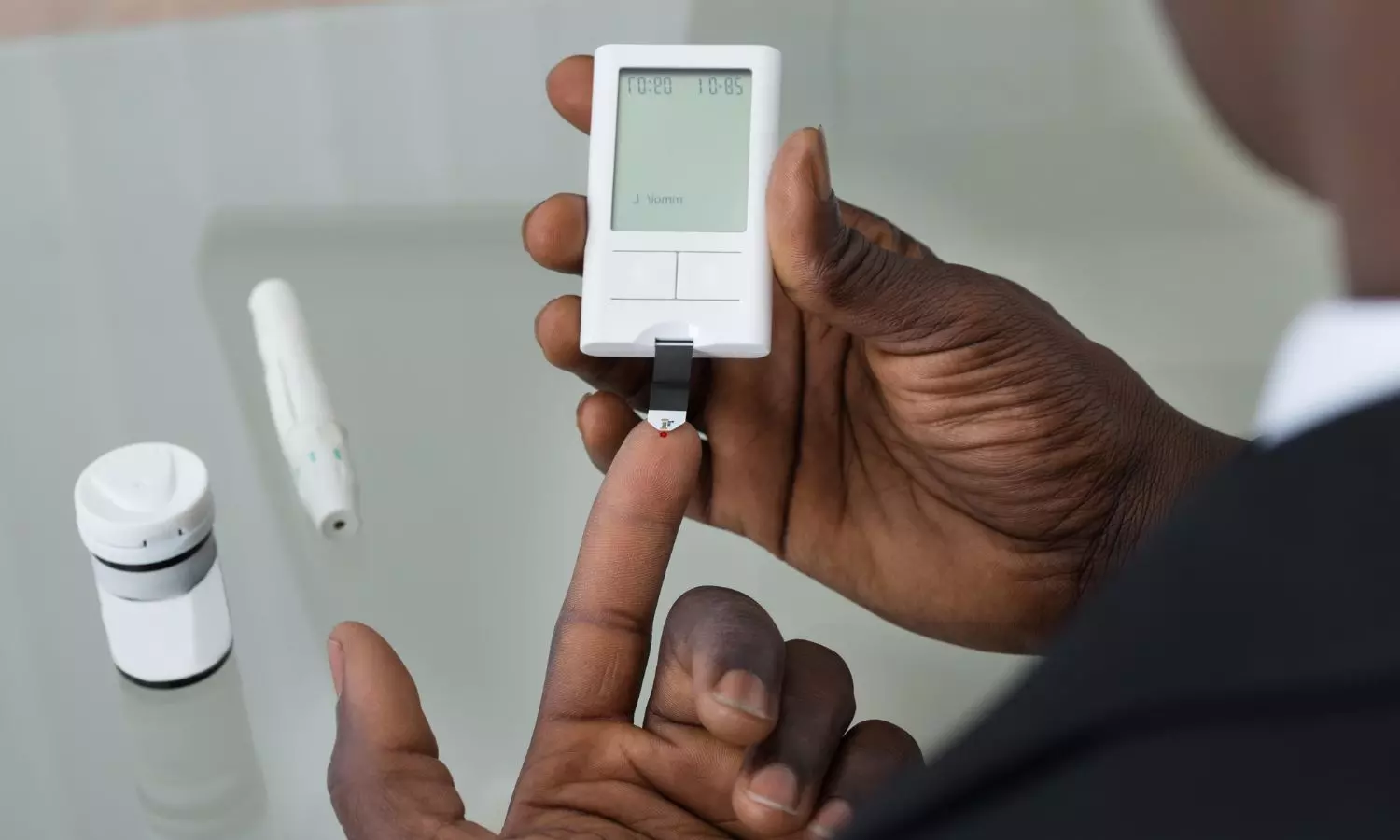
Research investigators reported that seizure in hypoglycemic patients seen in the emergency department (ED) was not significantly linked to a history of epilepsy. One prospective study of 32 institutions in Western Japan showed that seizures were seen in about 5% of hypoglycemic patients, but blood glucose was not significantly different between those with and without seizures. The study was published in the Acute Medicine & Surgery journal by Urushidani and colleagues. This result emphasizes that there can be other factors at play besides an epilepsy history in hypoglycemic patients that may influence seizure risk.
Hypoglycemia is a general medical emergency characterized by low blood glucose below 70 mg/dL that may be associated with serious neurological complications, including seizures. While severe hypoglycemia is an established cause of seizures, this relationship in non-epileptic patients with hypoglycemia is still relatively less certain. This study evaluated the characteristics and frequency of seizure events in hypoglycemia patients published in Acute Medicine and Surgery. It assessed whether a previous history of epilepsy could play a significant role in hypoglycemic patients developing seizure episodes.
This was a single-center, retrospective, observational study conducted at Western Japan from January 2017 to December 2021. Participants included all patients aged 16 years and above brought to the ED with symptomatic hypoglycemia. Data were extracted for blood sugar at first presentation, seizure at presentation, and other clinical variables from the final ED diagnostic records.
The primary outcome measure was the prevalence of seizures in patients with hypoglycemia. The secondary outcomes were comparisons between the initial blood glucose levels of the two groups with and without seizures, along with the analysis of related clinical factors. The statistical analyses were done using the Mann-Whitney U-test and the Fisher exact test.
Key Findings
Out of a total of 380 hypoglycemic patients, seizures were observed in a mere 5.0%, while all others patients failed to present with seizure activity.
Out of the 19 cases with a seizure, 12 were male and 7 were female. The majority of them manifested as generalized in.
The median initial blood glucose for the seizure group was 34 mg/dL; however, those in the nonseizure group exhibited initial blood glucose ranging from 37 mg/dL.
Initial blood glucose were similar for the seizure and nonseizure groups, (P= 0.97)
The most prominent disorder underlying seizure was reported among patients diagnosed with type 2 diabetes (n=8), type 1 diabetes (n=8), alcohol-related disease (n=2), and postgastrectomy syndrome (n=1).
Ten out of 19 seizure patients were hospitalized in comparison to 182. out of the 361 of the patients without seizure .
Among the group, 18 got intravenous Glucose treatment, one patient got oral treatment, and four patients were given Vitamin B1 treatment.
Three patients were treated with Diazepam, where 2 of them were given Diazepam to control the seizure and one for the sake of seizure control before the glucose examination. And none of the patients were administered the Glucagon treatment.
The score which was noted in the Glasgow Coma Scale was inferior in patients who had seizures (with a median, 10) as compared to those who had not presented with any seizures (with a median, 12). In a small number of cases, hospitalization was necessary; no mortality occurred in the cohort of patients with seizures.
The findings add important insight into the interplay between hypoglycemia and seizure occurrence in ED. Notably, the initial blood glucose levels of those with and without seizures did not have significant differences, suggesting probably that the severity of hypoglycemia alone might not be an adequate predictor for seizure risk. Other assumptions, like a history of epilepsy being a cardinal risk factor for seizures among hypoglycemic patients, found no strong correlation.
This study therefore shows that seizures in people with hypoglycemia are not majorly related to any history of epilepsy, and that there is no difference in the level of blood glucose between those who develop seizure conditions and those without such conditions at the time of presentation. The findings, therefore, call for further research into other determinants of seizure risk among hypoglycemic patients. Future studies with larger samples and more standardized methods for measuring glucose would be required in the management of these patients in the ED.
Reference:
Urushidani S, Tanabe M, Baek K, Miyaguchi K, Ikegami T. Seizure occurrences among hypoglycemic patients in the emergency department. Acute Med Surg. 2024;11(1):e979. doi:10.1002/ams2.979
Powered by WPeMatico

A new study published in the Journal of American Medical Association suggests that the risk of sudden death or resuscitated cardiac arrest (RCA) following an acute myocardial infarction (AMI) peaked in the first month and then quickly decreased.
The patients with pulmonary congestion and/or left ventricular dysfunction following an acute myocardial infarction were recruited for the Valsartan in Acute Myocardial Infarction (VALIANT) and Prospective ARNi vs. ACE Inhibitor Trial to Determine Superiority in Reducing Heart Failure Events After MI (PARADISE-MI) studies. In order to compare the rates of sudden death and resuscitated cardiac arrest following AMI in the PARADISE-MI and VALIANT trials, James Curtain and colleagues undertook this study.
The PARADISE-MI experiment enrolled participants between December 2016 and March 2020, while the VALIANT trial enrolled participants between December 1998 and June 2001. In the VALIANT and PARADISE-MI trials, the median follow-up was 22 months, while it was 24.7 months in the former. The research included individuals with AMI who were further affected by left ventricular failure or pulmonary congestion.
In the VALIANT trial enrolled 14,703 patients overall, the cohort was further refined to a subgroup that mirrored the risk profile of patients in the PARADISE-MI trial which was characterized by at least one augmenting risk factor and no prior history of heart failure. This subgroup comprised of 9,617 patients and reported a 7.4% incidence of sudden death or RCA. In contrast, the PARADISE-MI trial included 5,661 patients and showed a substantially lower incidence of 2.6%.
The analysis highlighted a particularly vulnerable period immediately following AMI, with sudden death rates peaking within the first month. Specifically, the rate of sudden death was 19.3 per 100 person-years in the VALIANT trial when compared to 9.5 per 100 person-years in the PARADISE-MI trial. These rates subsequently declined, illustrating the critical need for intensive early intervention post-AMI.
The reduction in sudden death rates in the PARADISE-MI trial can be attributed to several factors associated with contemporary management practices. The patients in the PARADISE-MI cohort were more frequently treated with percutaneous coronary intervention (PCI) for their initial AMI, a procedure that opens blocked coronary arteries and restores blood flow to the heart. Additionally, the use of β-blockers, statins, and mineralocorticoid receptor antagonists was more common in the PARADISE-MI cohort when compared to the VALIANT cohort. Overall, the risk of sudden death/RCA in patients with a decreased left ventricular ejection fraction and/or pulmonary congestion was shown to be 2 to 3 times lower in the individuals getting contemporary care when compared to their counterparts from two decades ago.
Reference:
Curtain, J. P., Pfeffer, M. A., Braunwald, E., Claggett, B. L., Granger, C. B., Køber, L., Lewis, E. F., Maggioni, A. P., Mann, D. L., Rouleau, J. L., Solomon, S. D., Steg, P. G., Finn, P. V., Fernandez, A., Jering, K. S., & McMurray, J. J. V. (2024). Rates of Sudden Death After Myocardial Infarction—Insights From the VALIANT and PARADISE-MI Trials. In JAMA Cardiology. American Medical Association (AMA). https://doi.org/10.1001/jamacardio.2024.2356
Powered by WPeMatico

The anti-obesity medication semaglutide may help to prevent heart attacks and other major adverse cardiac events among overweight people who have cardiovascular disease, whether or not they also have heart failure, according to a new study led by UCL’s Professor John Deanfield.
The results follow previous research from the same international team finding that weekly injections of semaglutide were linked to a 20% reduction in major adverse cardiac events (MACE) such as heart attacks and strokes for people with obesity or who were overweight and had cardiovascular disease.
The new study, published in The Lancet, found similar cardiovascular benefits for a subgroup of study participants who were also judged to have heart failure (i.e. whose hearts did not pump blood around the body properly) by a clinician at the start of the trial.
The researchers looked at data from 4,286 people – out of a total of 17,605 from the landmark Semaglutide and Cardiovascular Outcomes (SELECT) trial who were randomly assigned either semaglutide or a placebo – who were followed up over an average of more than three years.
They found that semaglutide was linked to a 28% reduction in major adverse cardiac events (12.3% in the placebo group had such events compared to 9.1% in the semaglutide group), as well as a 24% reduction in cardiovascular disease-related deaths for this subgroup of people with pre-existing heart failure, and a 19% reduction in deaths of any cause.
Lead author Professor John Deanfield (UCL Institute of Cardiovascular Science) said: “Our previous SELECT analysis showed the benefits of semaglutide for people with cardiovascular disease who had obesity or were overweight. This new study finds that, within this group, people with heart failure did just as well as people without in terms of the outcomes we measured.
“This is important as there were concerns that semaglutide might be harmful** for people with a type of heart failure known as reduced ejection fraction, where the heart pumps less blood around the body. Our findings show that the benefit of semaglutide was similar regardless of heart failure type.”
The study looked at data from the landmark SELECT trial-the largest and longest clinical trial of the effects of semaglutide on weight in over 17,000 adults who did not have diabetes but who were overweight or had obesity. The international team that runs the trial includes Professor Deanfield.
Semaglutide, a GLP-1 receptor agonist, simulates the functions of the body’s natural incretin hormones, which help to lower blood sugar levels after a meal. It was initially prescribed for adults with type 2 diabetes.
Semaglutide is the active ingredient in Wegovy and Ozempic. In July, thanks to evidence from the SELECT trial, the UK medicines regulator approved Wegovy as a treatment for those with cardiovascular disease, meaning it can be prescribed privately.
However, the drug is not yet recommended for this use in the NHS. Its benefits may first need to be compared to those of another new medicine, SGLT2 inhibitors, a diabetes drug also found to have cardiovascular benefits. (Wegovy is already available on the NHS to help with weight management and for people with type 2 diabetes.)
The exact mechanism through which semaglutide delivers cardiovascular benefits is not known, but may include the drug’s positive impacts on blood sugar, blood pressure, and inflammation, as well as direct effects on the heart muscle and blood vessels.
The researchers said the reduction in all-cause mortality in all heart failure groups “suggests the potential for other, as yet unknown, benefits”.
The study compared the impact of semaglutide for people with two types of heart failure: preserved ejection fraction, where the heart pumps blood normally but is too stiff to fill properly, and reduced ejection fraction. These two heart failure types have different causes and respond to treatment differently, with preserved ejection fraction, the most common type, not responding so well to traditional treatments, leading to considerable unmet clinical need.
The researchers found the clinical benefit of semaglutide was irrespective of type of heart failure. It was also found to be independent of age, sex, baseline BMI, and clinical status. Serious adverse events were reported more frequently in the placebo group than in the semaglutide group. Treatment was discontinued more often in the semaglutide group, primarily driven by gastrointestinal disorders (14.7% vs 9.0% in the heart failure groups; and 17.2% vs 7.9% in non-heart failure groups).
These findings, they said, supported the use of semaglutide, on top of usual care, to reduce the risk of major adverse cardiac events in a broad population of people with established atherosclerotic cardiovascular disease and overweight/obesity.
The researchers noted further trials were needed to evaluate the impact of semaglutide on heart failure-related outcomes. As SELECT was not a dedicated heart failure trial, the study results cannot be extrapolated to patients with heart failure in general, they said.
In their section on limitations, the authors noted that a majority of study participants were male and a high proportion were white. In future, they said, GLP-1 receptor agonist trials should examine responses by ethnicity and sex.
Reference:
Prof John Deanfield, Prof Subodh Verma, Benjamin M Scirica, Prof Steven E Kahn, Scott S Emerson, Prof Donna Ryan, Semaglutide and cardiovascular outcomes in patients with obesity and prevalent heart failure: a prespecified analysis of the SELECT trial, The Lancet, https://doi.org/10.1016/S0140-6736(24)01498-3.
Powered by WPeMatico

A study of fasting and the ketogenic diet reveals a new vulnerability of pancreatic tumors to an existing cancer drug.
Scientists at UC San Francisco have discovered a way to get rid of pancreatic cancer in mice by putting them on a high fat, or ketogenic, diet and giving them cancer therapy.
The cancer therapy blocks fat metabolism, which is the cancer’s only source of fuel for as long as the mice remain on the ketogenic diet, and the tumors stop growing.
The team made the discovery, which appears in Nature, while they were trying to figure out how the body manages to subsist on fat while fasting.
“Our findings led us straight to the biology of one of the deadliest cancers, pancreatic cancer,” said Davide Ruggero, PhD, Goldberg-Benioff Endowed Professor and American Cancer Society Research Professor in the Departments of Urology and Cellular Molecular Pharmacology at UCSF and senior author of the paper.
Ruggero’s team first uncovered how a protein known as eukaryotic translation initiation factor (eIF4E) changes the body’s metabolism to switch to fat consumption during fasting. The same switch also occurs, thanks to eIF4E, when an animal is on a ketogenic diet.
They found that a new cancer drug called eFT508, currently in clinical trials, blocks eIF4E and the ketogenic pathway, preventing the body from metabolizing fat. When the scientists combined the drug with a ketogenic diet in an animal model of pancreatic cancer, the cancer cells starved.
“Our findings open a point of vulnerability that we can treat with a clinical inhibitor that we already know is safe in humans,” Ruggero said. “We now have firm evidence of one way in which diet might be used alongside pre-existing cancer therapies to precisely eliminate a cancer.”
Humans can survive for weeks without food, in part because the body burns stored fat.
During fasting, the liver converts fats into ketone bodies to use in place of glucose, the body’s normal source of energy. Ruggero’s team found that eIF4E in the liver became more active, even as the liver paused its other metabolic activity, suggesting that this factor was involved in making ketone bodies, a process called ketogenesis.
“Fasting has been part of various cultural and religious practices for centuries, often believed to promote health,” said Haojun Yang, PhD, post-doctoral researcher in Ruggero’s lab and first author of the study. “Our finding that fasting remodels gene expression provides a potential biological explanation for these benefits.”
By tracking how different metabolic pathways changed during fasting, the scientists discovered that eIF4E was activated by the presence of free fatty acids, which are released by fat cells early in fasting, so the body has something to consume.
“The metabolite that the body uses to make energy is also being used as a signal molecule during fasting,” Ruggero said. “To a biochemist, seeing a metabolite act like a signal was the coolest thing.”
These same changes in the liver — ketone body production from burning fat, along with a rise in eIF4E activity — also occurred when laboratory animals were given a ketogenic diet consisting mostly of fat.
That’s when the lightbulb went off.
“Once we could see how the pathway works, we saw the opportunity to intervene,” Ruggero said.
The scientists first treated pancreatic cancer with a cancer drug called eFT508 that disables eIF4E, intending to block tumor growth. Yet, the pancreatic tumors continued to grow, sustained by other sources of fuel like glucose and carbohydrates.
Knowing that pancreatic cancer can thrive on fat, and that eIF4E is more active during fat burning, the scientists first placed the animals on a ketogenic diet, forcing the tumors to consume fats alone, and then put them on the cancer drug. In this context, the drug cut off the cancer cells’ only sustenance — and the tumors shrank.
Ruggero, along with Kevan Shokat, PhD, UCSF professor of cellular and molecular pharmacology, developed eFT508 in the 2010s, and it showed some promise in clinical trials. But now, there’s a much more powerful way to use it.
“The field has struggled to firmly link diet with cancer and cancer treatments,” Ruggero said. “But to really connect these things productively, you need to know the mechanism.”
Different diet-drug combinations will be needed to treat more forms of cancer.
“We expect most cancers to have other vulnerabilities,” Ruggero said. “This is the foundation for a new way to treat cancer with diet and personalized therapies.”
Reference:
Haojun Yang, Vincenzo Andrea Zingaro, James Lincoff, Harrison Tom, Satoshi Oikawa, Juan A. Oses-Prieto, Quinn Edmondson, Ian Seiple, Hardik Shah, Shingo Kajimura, Alma L. Burlingame, Michael Grabe, Davide Ruggero. Remodelling of the translatome controls diet and its impact on tumorigenesis. Nature, 2024; DOI: 10.1038/s41586-024-07781-7
Powered by WPeMatico

Human skin, hair and nails are all vulnerable to fungal infections. While these infections are usually not serious, they’re difficult to fully resolve and often recur after treatment-sometimes for years. They’re also often resistant to treatments, including a common class of antifungals called azoles.
A study published this week in mSphere mSpherepoints to a new way to boost the efficacy of azoles in treating those infections-combining them with commonly available drugs called bisphosphonates, usually used to treat osteoporosis. Previous work by the same research group has shown that adding bisphosphonates to azoles can effectively treat yeast infections from Candida and Cryptococcus species. The new study extends that finding to dermatophytes, which cause superficial infections.
The study suggests that bisphosphonates could be repurposed to use with azole antifungals, which are relatively nontoxic, and that the combination could be readily tested in clinical studies.
“There aren’t many good antifungal drugs around, and the fungus will always develop resistance no matter how you treat them,” said senior author Dee Carter, a mycologist at the University of New South Wales, Australia. “For what we’re proposing, to use 2 drugs at the same time, that resistance is much less likely.”
Carter says she was only a little surprised to see the synergistic effect in dermatophytes. This research project began years ago, she says, when her group conducted a series of genomic analyses on the response of pathogenic yeasts to drug treatment. That study led them to a genetic pathway that is “upstream” of the pathway targeted by azoles, and is instead targeted by bisphosphonates. “That’s often a good way to get drugs to work, is to target processes that are interlinked like that,” Carter said.
In the lab, Carter and her team tested 3 commonly available bisphosphonates (risedronate, alendronate and zoledronate) in combination with 3 commonly available azole antifungals (fluconazole, itraconazole and ketoconazole). They tested these against clinical isolates from a diverse range of dermatophyte species that cause superficial infections. The combination of zoledronate and ketoconazole proved particularly effective against 8 of the 9 tested species. It also prevented the development of resistance.
Aidan Kane, mycologist, lead author of the study and a Ph.D. student in Carter’s lab, used fluorescence microscopy and other methods to show that the drug combination worked by weakening the cell membrane enough that the fungus could not survive. Beyond the dermatophytes, the group also found that bisphosphonate-azole combinations could act against molds that cause invasive disease, suggesting another possible clinical application for the drugs.
“You can use these combinations directly for superficial infections, like Candida or dermatophyte infections, and we’re hoping that with modified forms of the drugs we can create something that will also work systematically,” Carter said. “The next step is to continue testing bisphosphonate-azole combinations in animal models, and then test it in clinical trials.”
Reference:
Aidan Kane et al, Bisphosphonates synergistically enhance the antifungal activity of azoles in dermatophytes and other pathogenic molds, mSphere(2024), DOI: 10.1128/msphere.00248-24.
Powered by WPeMatico
